Sponsored by: AscendRural

AscendRural’s Senior Care Accelerator is accepting applications through this Friday, January 9th for pilot-ready solutions that support aging populations in rural communities.
Their four-week program helps early stage startups pilot, validate, and scale solutions, in real rural settings with the opportunity to secure funded pilot contracts worth up to $150k.
Selected teams will also gain mentorship, rural market insights, structured readiness support, and connection to AscendRural’s ecosystem of national and regional partners.
If you're interested in sponsoring the newsletter, let us know!
Welcome back from what was hopefully a restful holiday season. It was a relatively quiet few weeks in healthcare news over the holidays, which I’m sure will change quickly this week as everyone gears up for JPMorgan the following week. Stay tuned for another note from us this week about some pop-up coverage I’ll be doing for the company presentations at JPM this year.
- Kevin
My Reflection: Arts and crafts and business
A question I’ve been asked a bunch of times over the years is why I don’t automate more of the newsletter creation process. It’s not hard to sketch out how much of what I do each week could be automated, saving me a bunch of time in the process. Yet I’ve always resisted the urge to automate this process.
Don’t get me wrong, there are certainly some Sundays that I’d rather not wake up at 5am to write a newsletter, as much as I enjoy the banter with y’all. But the primary reason I haven’t is a selfish one — the act of creating this newsletter is a bit like my own personal art project that I get to do each week. Each newsletter is a puzzle I get to solve; an opportunity to hone my craft. I’ve learned to cherish the opportunity to think deeply in this way each week.
As our various worlds are consumed by AI-generated everything, I believe the craft that goes into things like this newsletter will increasingly stand out. A blog post over the holidays by Scott Belsky suggested something similar, discussing among other things the importance of the craft that goes into products in 2026. I am obviously biased, but it definitely resonated with me.
You might ask, ok Kevin, but what does any of this have to do with healthcare? Well, I thought this point below from Belsky’s post about a movement towards more “front of house” humans is quite relevant:
It was particularly interesting to see this sentiment given how much of the healthcare AI innovation in 2025 seemed focused on automating away what have historically been awful “front of house” patient experiences.
I covered it extensively in newsletters in 2025 — from Doctronic's growth as an AI symptom checker to Assort Health's adoption as an automated phone tree for practices to Hippocratic AI's handling of outbound calls for health systems, there seems to be abundant enthusiasm for funding efforts to automate healthcare’s “front of house” experience. The business imperative behind this seems clear — expanding operating margin via reduced labor costs is a meaningful lever for care delivery organizations. And when the status quo bar is so low, it presents an easy near-term opportunity to improve upon.
WellSpan Health’s CEO articulated the vision of their partnership with Hippocratic AI well here back in October, providing a sense of how it supports that business imperative:
Our vision right now is we want care anytime, anywhere, and we think that that's how people are going to consume health care in the future. So Anna could be a huge part of that, and we've already considered her a part of our care team.
So she gets introduced as our AI care assistant. Patients interact with her, but a vision for the future could be around every person who reaches out to WellSpan is initially greeted by Anna. That she really is our front door for any call or any contact — Web, phone, anything. And she's doing a terrific job so far. We've made over 1.6 million calls with Anna. She's a very hard worker. And this last week she scheduled more than 50% of our primary care visits for the week. Clearly, by completing that scheduling, patients enjoy interacting with Anna or they wouldn’t complete the call.
Yet while reading that, I can’t help but wonder whether this vision of automating every interaction is the wrong direction for care delivery organizations to head. Thinking about Belsky’s thesis, these automated interactions will feel cheap and drive a poor experience. The reaction on Facebook to Hippocratic’s deployment at WellSpan already provided a glimpse of this. People will choose experiences with human touch when given the opportunity. Case in point: if you look at the website of a high-end concierge experience like Private Medical, the primary value prop is direct access to your physician at any time, not the quality of the LLM you get to interact with.
So if I apply Belsky’s hospitality thought bubble to healthcare’s front door, I think a more interesting vision from a care delivery organization would be one in which there is no longer any need for a patient to interact with a symptom checker, listen to an automated phone tree, or receive an automated message in the first place. Giving patients convenient access to a personalized, human experience? What a world that would be!
There is obviously an important role for AI and technology to enable that experience at a price point more affordable than today’s oncierge experience. But rather than just automating away human interactions to save on labor costs, it blends into the background of a fundamentally human experience. The arbitrage opportunity of replacing labor with robots will close quickly. Particularly in an industry where so much is driven by human relationships, figuring out how to enable this experience — at an acceptable margin — seems mission-critical.
So, whether you’re a creator like me or running a care delivery organization, I think we’re all going to be thinking a lot about how AI supports, rather than automates away, the humanness and craft that goes into our respective products in 2026.
Community Discussion Topic: Is VBC Succeeding?
You may recall that back in November, I highlighted a conversation between Aledade’s Farzad Mostashari and Brown’s Andrew Ryan, in which they took opposite sides answering this question. Mostashari made a solid defense of the principles of value-based care and the success of the MSSP program. Ryan’s argument against VBC was light on details but nonetheless effective in planting the seed that it might be time to move on from VBC as a mechanism to cure what ails American healthcare. If nothing else, the conversation underscored the divergence of opinions on the topic.
As we enter 2026, it seems this will be a pivotal year for the momentum of value-based care. Given this, I thought it’d be a good conversation to unpack more this week in the community, starting with the poll below:
After fifteen years, is value-based care succeeding?
For HTN Community Members:
One of the things we’re excited to spend more time on in the community in 2026 is to focus conversations on a set of topics we think are particularly impactful to learn about together. As we experiment with how best to support this, we thought we’d kick off the year with an ongoing discussion about the VBC question above.
During the week, we’ll post a few prompts for community members to discuss with articles that have spurred our thinking on a new channel specific to this topic. On Thursday, I’ll host Aledade’s Co-Founder, Farzad Mostashari, for a conversation about Aledade’s recently announced credit facility and his broader perspective on financing value-based care. On Friday, we’ll wrap up the week by hosting a discussion for community members to share learnings on the topic.
If you’re looking to think more about the current state of VBC this week, we’d encourage you to sign up here:
Chart of the Week: BCBS VT’s transparency push
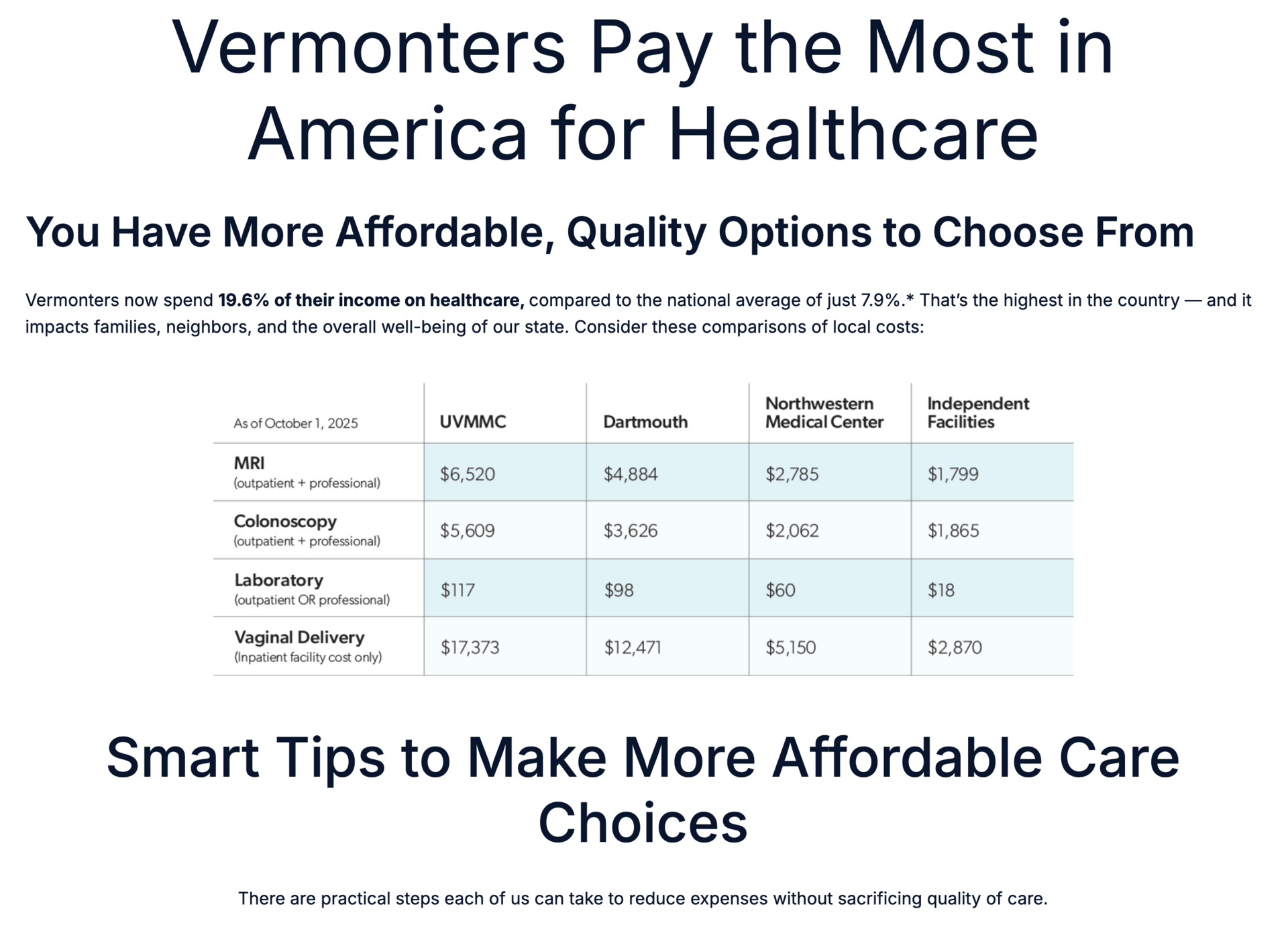
Blue Cross Blue Shield of Vermont took a rather bold step this week in attempting to drive utilization away from a high-cost academic medical center in Vermont. It launched a website, Vermont Affordable Care, in partnership with four lower-cost provider organizations, attempting to help Vermonter’s understand what services cost at various locations. It’s an interesting effort to use cost data to try to influence where Vermonter’s seek care:
Several Blues plans over the last several months have taken to the public arena to discuss the high costs of healthcare — see recent BCBSM or BCBSNC op-eds as examples. This effort stands out for how it calls out the market-dominant provider, the University of Vermont Medical Center (UVMMC). The local news coverage provides a good hint as to why this is out of the norm — BCBS VT is walking a tightrope, trying to steer people away from UVMMC while also ensuring UVMMC doesn’t get so upset that it leaves the network.
In general, I remain pretty skeptical that price transparency will actually help reduce costs. The basic reasoning being that high-priced providers will stay high because they can, while lower-priced providers will use those higher prices to justify higher prices for themselves. See the results of the No Surprises Act or the North Carolina State Health Plan’s Clear Pricing Project as examples.
But if transparency can help reduce costs, I think it’ll be through efforts like this one from BCBS VT. Kudos to them for pushing the boundaries here, I’m hopeful it’ll help reduce costs in that market.
Other Top Headlines
CMS announced the 2026 funding awards for the $50 billion Rural Health Transformation Program. $10 billion will be doled out to all 50 states in 2026, with Texas and Alaska leading the way at $281 million and $272 million, respectively. New Jersey received the lowest award at $147 million. If you do the math on a per capita basis for the rural population in each state, Rhode Island is far and away the leader, while Texas is actually at the bottom.
Prenuvo and a radiologist are facing a malpractice lawsuit from a patient who suffered a stroke after receiving a Prenuvo scan in 2023. The lawsuit argues they missed major warning signs that could have prevented the stroke and instead indicated results were normal. While the case is ongoing, a judge denied Prenuvo's effort to cap the medical malpractice amount under California law. It appears that Prenuvo’s radiologist involved in the case also separately pleaded guilty in January 2024 to participating in a $70+ million insurance fraud scheme in New York. Perhaps it’s just me, but this seems like a pretty concerning data point that contradicts a lot of the cutting-edge technology narrative from Prenuvo’s $120 million funding announcement in early 2025.
The FDA approved Novo Nordisk’s oral pill version of Wegovy.
Funding Announcements
TrueMed, a marketplace for spending HSA / FSA benefit dollars, raised $34 million. a16z led the round. Given the growing interest in longevity offerings and political support for HSA accounts, it seems TrueMed is well-positioned to ride a wave in this market.
What I’m Reading
Town Hall Ventures’ 2026 Predictions by Andy Slavitt, Josh Loria, & Andie Steinberg
I’ve avoided most 2026 predictions articles, but I thought this one had some interesting perspectives, particularly on the policy landscape. Specifically, I thought the discussion of CARA as a key piece of CMMI’s new LEAD model was particularly interesting, noting it could lead to a meaningful uptick in sub-capitation models.
Read more
Mark Cuban Tells Us How He Can Fix America’s Sh!tty Health Care by Jonathan Cohn
Mark Cuban is all over the place these days sharing his perspectives on how to f*ck up fix healthcare. I thought this was a good interview between him and Jonathan Cohn in The Bulwark, featuring some of these thoughts. I’d share Cohn’s sentiment in the post that some of the things that Cuban says make sense, and some don’t. It seems like a rather polite way of characterizing the coherence of the general narrative.
I must admit, this narrative feels a bit like Groundhog Day — if you’ll recall, I also kicked off 2025 sharing my frustrations with another blog post from Cuban. One new thing I did learn over the holidays this year is that Mark Cuban actually came up with his own plan for financing healthcare in this country a few years back, called the 10Plan. Cuban certainly deserves credit for the impact that Cost Plus Drugs has had, but the general oversimplification and finger-pointing seem deeply unhelpful in actually moving the conversation forward productively. The failure to gain traction Cuban has experienced on efforts like the 10Plan or Cost Plus Wellness (not to mention his desire to partner with Humana on Cost Plus Drugs) surely indicates he’s more aware of the complexity here than he leads on in conversations like this one, where it comes across like he thinks virtually everyone else is an idiot, or evil, for not having fixed healthcare already.
Read more
Featured Jobs
Senior Associate, Strategy & Operations at Hopscotch Primary Care, delivering tech-enabled primary care to rural communities. Learn more.
Chicago (hybrid)
Director of Operations at TotalCare, providing tech-enabled primary and urgent care to underserved communities in southern CA. Learn more.
$175K - $250K | In-person (Chino, CA)
Director of Customer Success at Oler Health, software that streamlines clinical documentation review. Learn more.
$100K - $150K | Remote (25% travel)
Technical Product Manager at SimpliFed, a virtual maternal health model. Learn more.
Remote
Customer Ops at Vitalize, automating staffing, scheduling, flow, and capacity for health systems. Learn more.
$150K – $240K | Hybrid (SF)
Contact us to feature roles in our newsletter.
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.