Sponsored by: Ketryx
Join Ketryx next Thursday, April 9th for the Validated AI Conference, a free, half-day hybrid event for operators and leaders to learn how AI is validated and applied in regulated environments.
Expert-led sessions will cover practical approaches to AI validation, compliance, and regulated product development, featuring leaders at Johnson & Johnson, KPMG, AcuityMD, Transformation Capital, and more.
Attend virtually or request a ticket to attend in-person at The Engine, MIT’s venture firm in Cambridge, via your confirmation email. Register here.
If you're interested in sponsoring the newsletter, let us know!
We’re taking next week off from the newsletters, which means I’ll be back on April 16th. If you miss us, tune into The Grand Round-Up, our weekly live show on Mondays at 12p eastern on LinkedIn, Youtube, or X.
Probably, the MA Final Rate Notice will drop Friday evening, but if it happens when we’re live, it would make for some great live streaming!
—Martin
Washington, D.C.
We talk a lot about adverse selection around here. If you’re a health insurance company, you want to insure, at most, a normal amount of sick people and not an unusually high number of sick people. If you end up with an unusually sick risk pool, there might have been some adverse selection where the healthy people didn’t buy insurance, or didn’t buy your insurance, and you got stuck with lots of bad risk or as is sometimes the case, good risk that goes bad.
This is a known issue, and there are lots of ways insurers and policy makers try to avoid adverse selection so insurance companies can compete on price, creative plan design, and networks: limited open enrollment periods, individual mandates, and cetera
But these aren’t laws of physics, and sometimes you end up getting the fuzzy end of the lollipop. And, if you’re a regulator, for market stability and social utility, you might want some mechanism to encourage insurance companies and other risk-bearing entities like ACOs to take on sicker members, or at least feel confident that if they end up with a sicker-than-average risk pool, they won’t get blown up.
For ACA plans, the risk adjustment mechanism is pretty tidy: the plans with healthier than average members pay the plans with sicker than average members, and it all nets out to zero.
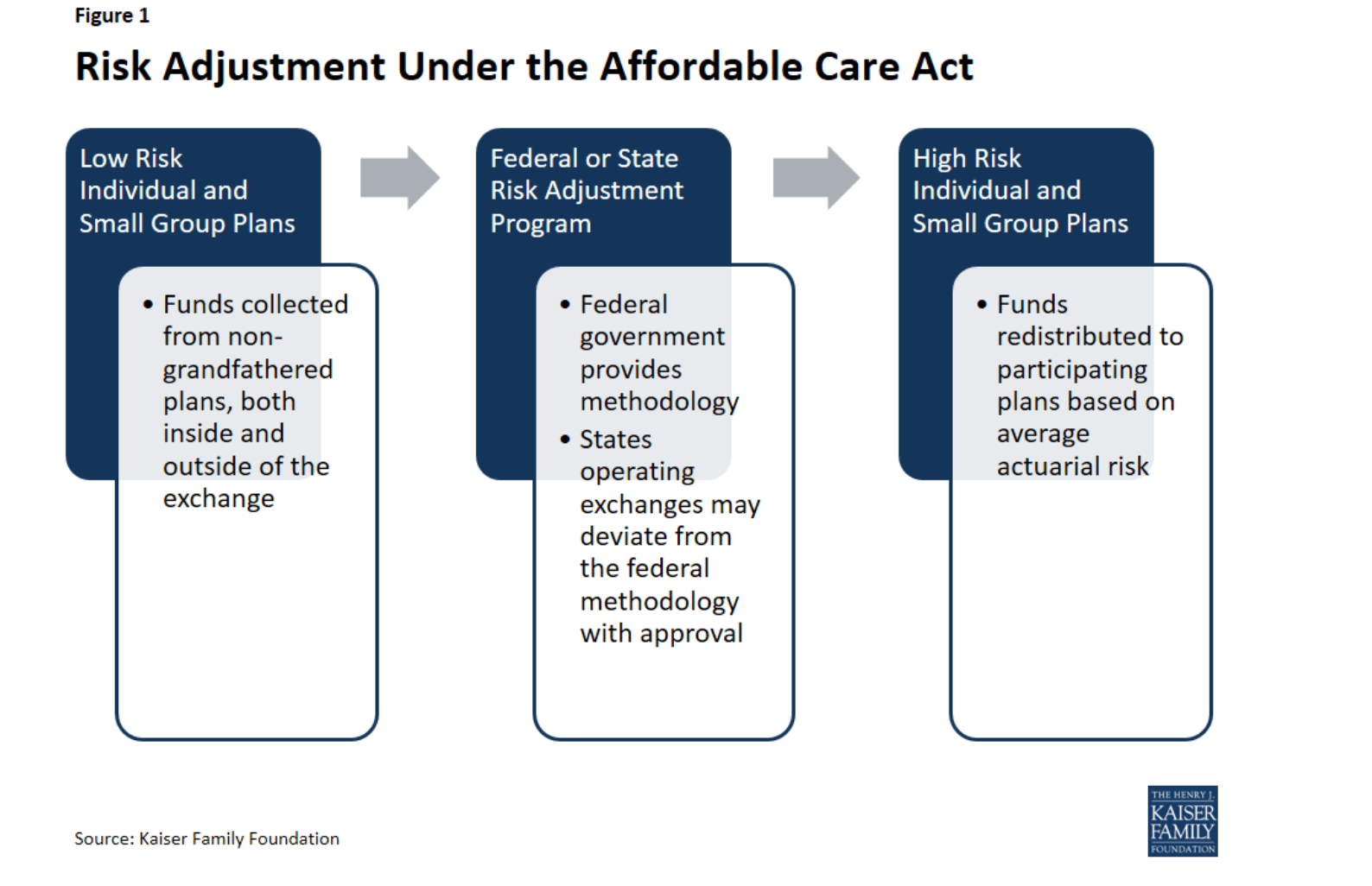
It’s conceptually similar for Medicare Advantage plans, but mechanically different in a couple of important ways, one of which is that, unlike in the ACA risk adjustment scheme, risk scores don’t net out to zero, resulting in a Lake Wobegon situation where all the MA members are above average, in terms of risk. The popular theory behind why this is is that risk adjustments are more or less self-reported to CMS by the plans, so there’s some incentive to “upcode” patients. This is hotly contested by MA plans who say they are just capturing the reality of insuring for what is, in their view, a sicker population.
For ACOs participating in the Medicare Shared Savings Program, risk scores are used to adjust the savings benchmark but, to prevent upcoding, the benchmarks don’t change if the risk scores increase during participation, which might lead to ACOs avoiding sicker patients. Not ideal!
Another ACO program, REACH, is spiritually closer to Medicare Advantage risk adjustment and its benefits and drawbacks, but the program is getting sunsetted and replaced by the Long-term Enhanced ACO Design (LEAD) model, whose RFA was released this past. There are a lot of moving pieces here, as demonstrated by this graphic:
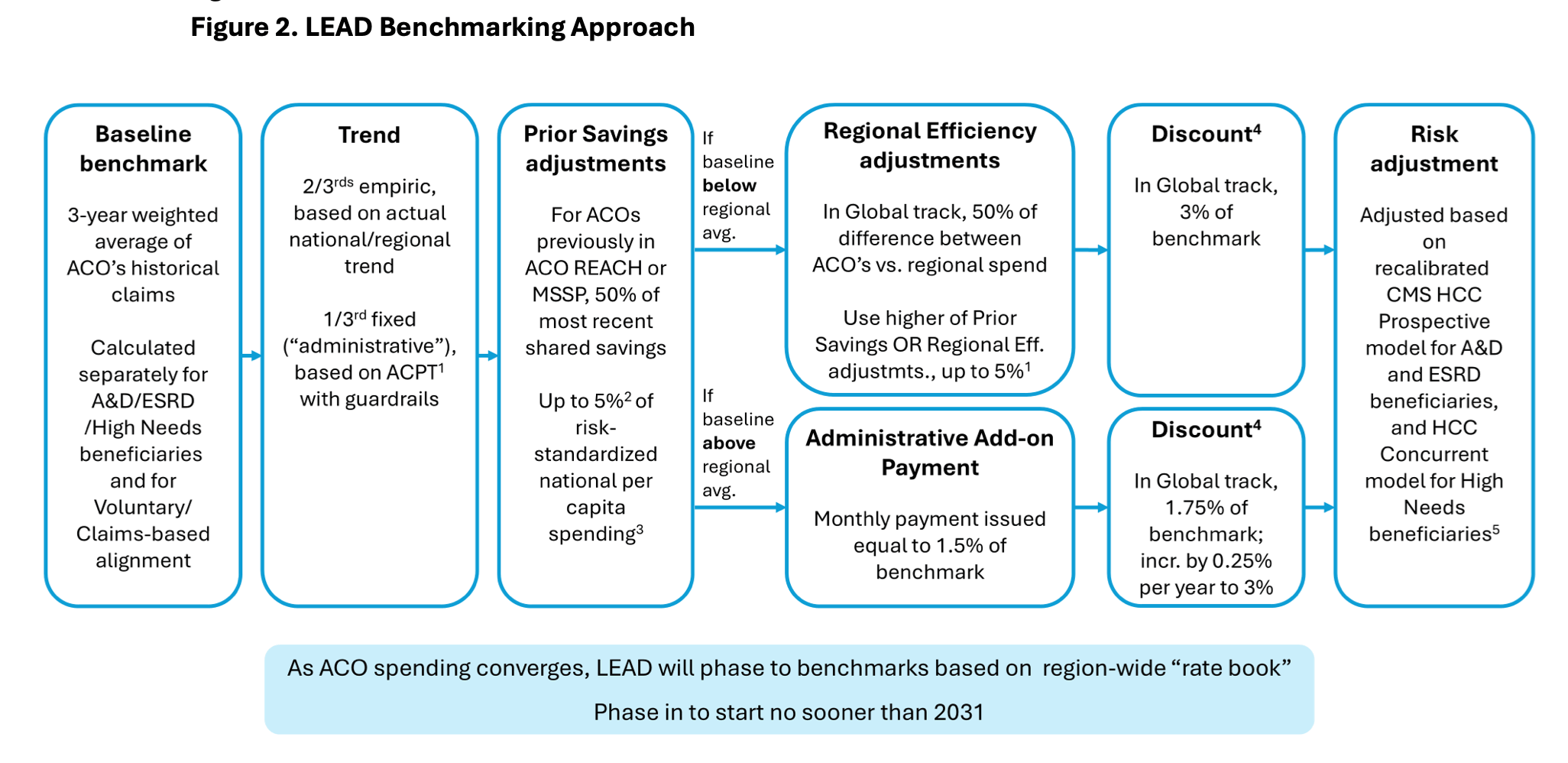
Perhaps most interestingly, in addition to the risk adjustment scheme described above, CMMI notes in a section titled AI-inferred risk adjustment that LEAD, “will shadow test the use of risk scores generated from an AI-inferred risk adjustment model for the A&D population.”
What’s inferred risk? Glad you asked. Conveniently, CMMI Director Abe Sutton and COO of Pearl Health Gabe Drapos wrote a whole Health Affairs Forefront article on the subject back in 2024:
CMS can analyze the enormous amount of billing data that flows through its systems and assign every patient a risk score. For instance, a patient with a history of office visit claims with a rheumatologist as confirmed by the provider’s CMS Specialty Code, an ongoing prescription for a Tumor Necrosis Factor (TNF) blocker (such as Humira/adalimumab), and pathological lab claims for relevant testing are a constellation of features that are nearly confirmatory of a rheumatoid arthritis diagnosis. CMS can aggregate such inferences across services rendered, labs performed, and medications filled to create a synthesis of diagnoses for a given patient, without gathering additional data. Diagnoses can continue to be mapped to expected costs and RAF scores, where populations of similar demographic and utilization factors – a “synthetic cohort” of similar patients – can provide actuarial confidence in costs.
While there will undoubtedly be statistical noise (such as false positives or overlooked diagnoses) at the individual patient level, at population sizes relevant to the use cases for RAF – the size of a small health plan’s membership, or the minimum ACO beneficiary pool (5,000 lives) – Medicare can accurately capture the expected disease burden and level of spend for that population.
CMS is sitting on a bunch of data between services, labs, and medications, and the idea here is to make inferences about the risk of members based on that data rather than relying on the old ways, at least for the LEAD model. Risk adjustment schemes always have trade-offs, and surely this one will have winners and losers, but it’s an exciting experiment to see if we can get more in the way of insurance market stability with less in the way of gamesmanship.
Elsewhere in Washington:
A bipartisan bill to limit downward pressure on Medicare Physician Fee Schedule was introduced in the House of Representatives
Dr. Oz’s Medicaid diagnosis, “The real problem in Medicaid is that we are paying for things that your family used to do for you.”
In what was surely not what congressional Republicans hoped for in terms of a headline, Axios wrote “GOP weighs health care cuts to pay for Iran war”
CMMI shared Kidney Care Choices PY 2024 financial performance, and Tim Fitzpatrick dug into the results
Wesley Sanders at Evensun gives his perspective on the 2026 ACA Open Enrollment file
State Capitols
If you’re a state legislator, what should you do with a $1 billion surplus? There are lots of defensible ways to answer this question. One answer might be: return it to your state’s taxpaying residents. You collected more than you spent, so you should give it back. Another plausible answer is that you should put it in a rainy day fund because there may be a reversal of fortune in the near future. A third answer is that you should spend it on investments, programs, and services that benefit your state and its residents.
Or you could do some combination of the three: refund a bit, save a bit, and spend a bit. Different people have different opinions, there’s no perfect answer, and these are the tough calls we elect politicians to make.
Health care is expensive in this country, and Medicaid in particular is a large line item for most state budgets, so if you, as a state legislator, were feeling flush with cash because of your surplus and some one-time transfers from the federal government, you might decide to spend more on your Medicaid program.
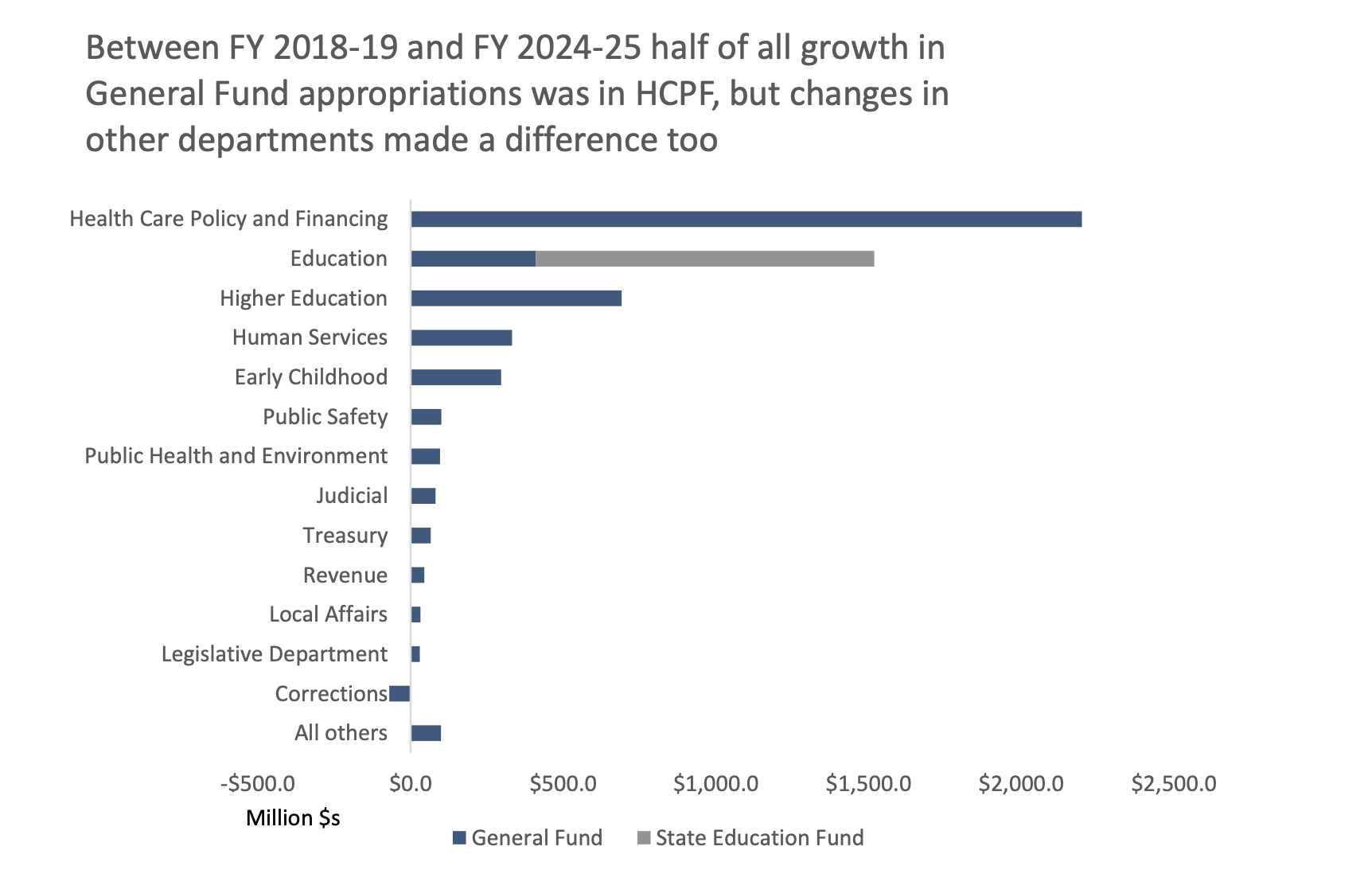
What would you spend it on? You might give some Medicaid providers a raise in the form of higher reimbursement ($114 million in FY 2023-24 and $125 million in FY 2024-25). Long-term services and support costs might increase a bit, from “by 44.0 percent from FY 2020-21 to FY 2023-24, from $2.9 billion to $4.1 billion.” There are children and pregnant mothers in your state who would be eligible for Medicaid but for their immigration status who you want to cover which your fiscal analysts project would cost $34.0 million but ends up being about looking closer to $60.3M for FY 2027-28. You might up the nursing home facility reimbursement rate to help ease the access crisis ($30.5 million in general funds). And on top of all of that, you might pass ~14 bills related to child welfare and mental health, all hard to argue with, at a cost of $71 million in general funds.
It could be a worsening fiscal situation at the state level, it could be dramatic changes to how the federal government finances Medicaid, but if the situation changes, you as a state legislator are going to have to make some tough calls. Like doubling the waitlist from 7 years to 14 years for 24/7 support for adults with developmental disabilities, a savings of $6.6 million or saving a few million in general funds by capping the number of hours family members can get reimbursed for providing care to a disabled dependent. Then there’s the reversing reimbursement increases or outright reimbursement cuts for Medicaid providers, and the imposition of limits on the Cover All Coloradans program for undocumented children and pregnant mothers.
Colorado’s state budget is exceptional in some ways due to its limits on taxation, but my sense in talking to folks at state Medicaid agencies is that it isn’t unique. Conversations like the one the Joint Budget Committee just finished will be happening in state capitols across the country. A lot of it is driven by the OBBBA changes to Medicaid financing, but it’s also emblematic of the broader health care conversation in Medicare and with employers. It’s expensive, and people don’t want to pay more, but paying less involves making some exceptionally hard choices.
Also happening at the state level:
New Jersey Governor Mikie Sherrill included $10 million in her proposed budget for Medicaid enrollment improvements
Colorado Medicaid Director Kim Bimestefer resigns effective April 10th after the state Senate circulates “no confidence” resolution, which as a former employee of Kim’s, I find incredibly disheartening. She was one of the greatest to ever do it in my own biased opinion.
Progressive think tank the Fiscal Policy Institute claims to find a basic math error in Dr. Oz’s fraud letter to New York State Medicaid
An op-ed from friend of HTN Lawson Mansell advocates for Pennsylvania to allow international doctors to practice in the state
More from Health Tech Nerds
Weekly Health Tech Reads
3/29/26: A musing on the peptide craze, a dozen different startup funding announcements, and more. Read here.
HTN Radio
Every Monday: The Grand Roundup Live
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.