I spent the first part of the week at AHIP’s 2026 Medicare, Medicaid, Duals, and Commercial Markets Forum. I was there mostly to listen to what the folks from CMS had to say, and if you’re a paid HTN community member you can read my summaries of the talks in the links below:

While it was pretty standard conference fare in terms of the speeches, it was interesting to hear the folks at CMS talk in and around the tension of health plans being a vital partner for CMS in managing costs, while at the same time communicating the higher expectations and tougher policy and financing environment they’re in for resulting from this administration’s policies. I’ve been impressed with this CMS leadership, and think they did a good job of walking this particular tightrope, but there was something of a pall over the whole event as the industry waits for the final rate notice, which is at OMB, and further guidance on Medicaid work requirements.
In the meantime, today I’m thinking about Medicare Director Chris Klomp’s proposal on auto enrollment in either MA or an ACO and the state of Nebraska’s proposal to end retroactive enrollment in Medicaid.
—Martin
Washington, D.C.
When you turn 65, there are a lot of different directions you can take your Medicare coverage. The two main avenues, however, are (1) traditional or original or Fee For Service Medicare and (2) Medicare Advantage. The basic trade-off you make between one or the other, as a consumer, is around monthly premium costs, network, and supplemental benefits like vision or hearing.
Health insurance is, at its core, a financial product, and like a lot of financial products, idiosyncratic needs and preferences will dictate whether original Medicare or MA is a better choice for you, individually.
What’s better for the government and its taxpayers, though? No one really knows, but people sure do like to argue about it! But the person whose view on this question is the most important is Chris Klomp, the Chief Counselor of HHS, Deputy Administrator of CMS, and Director of the Center for Medicare, and last week at a STAT conference, he made some news:
CMS has a stated goal and this precedes the Trump administration, the Biden administration and beyond that every beneficiary, being an accountable relationship. Why do we care about that? We just talked about it because accountable relationships lead to higher quality measures, a better clinical experience, better clinical performance. It's healthier beneficiaries, healthier patients. And so could we see a default selection into an accountable relationship, which could be an ACO through the Medicare Shared Savings Program or a derivative or successor CMMI model from the Center for Medicare and Medicaid Innovation led by Director Sutton? Yes. Could it be through a Medicare Advantage enrollment? Yes.
Would either of those, in my view, be superior to a default enrollment into a fee-for-service arrangement where there's not this long-term secular relationship between the beneficiary, the patient and their provider? Yes. Why? Because we see healthier beneficiaries. That's a good thing.
Kevin talked about this in his newsletter, and I heard some variations on the theme from Klomp and Oz at AHIP. A lot of the headlines that were sparked by this comment, including Mario’s, were about the specter or prospect, depending on your opinion, of automatic enrollment in MA plans:

To riff on what Kevin wrote this weekend, a more generous interpretation is that Klomp et al are focused on getting everyone in a managed care relationship. MA is one way to do that, and between the advanced rate notice and the speech Klomp at AHIP on stewardship of taxpayer dollars and gamesmanship of risk adjustment, my view is that in sum, this might not be viewed as all that great a “benefit” for major health insurance companies. But these headlines also ignore the potential tailwind for ACOs who are “cautiously supportive of an idea floated by CMS’s Medicare chief to automatically enroll beneficiaries into Accountable Care Organizations.”
There is still a lot of work to be done on the MA side to make them good stewards of patients’ health and the nation’s finances, and there’s still quite a bit to be done on the ACO side as well, but I like Klomp’s theory of the case here which to me reads as: we’ve got two structures to manage care and costs for Medicare, and those paths, MA or ACO should be the default. Those structures may need some improvement, but they’re better than no care management structure at all.
Also in Washington, D.C., effectuation rates for ACA are imminent, Milliman on the CMMI lead model and dual-eligibles, Cityblock CEO Toyin Ajayi on AI and Medicaid, CMMI announces the ASPIRE (Accelerating State Pediatric Innovation Readiness and Effectiveness) Model, and v28 had a limited impact on Medicare Advantage benefits, study finds.
State Capitols
Something insurers worry a lot about is adverse selection. If you’re on the hook for covering some or all of a person’s medical costs, like an insurance company is, you want a good mix of mostly healthy people and fewer sick people. This is one reason why the ACA included an individual mandate, which was effectively a penalty in the form of a tax for not having insurance, and, more generally, why health insurance products have restrictive enrollment periods.
In the absence of a penalty and restrictive enrollment periods, the healthy people, or people who think they’re healthy, might say, “I don’t really need to pay for insurance, and if I get sick, I’ll just go out and buy it.” This would be bad, specifically, for the insurers, but also bad on a societal level, because it would be hard for insurance companies to stay in business, and then no one could have insurance.
So, in general, to avoid adverse selection, an insurance company won’t let you buy insurance only when you need it. But there are exceptions! One odd one is the COBRA law, which allows you to keep your insurance after you leave a job and also gives you a 60-day grace period to pay the first premium. So you could, in theory, on your way to the hospital on the 59th day in the back of the ambulance, pay your premiums and get covered if something bad happened, or not pay them, if nothing bad happens. This leads to a meaningful amount of adverse selection in this corner of the insurance market.
Another area where you can get coverage retroactively, which is just pure adverse selection, is in Medicaid, which explicitly allows for retroactive coverage for up to 90 days, though states can apply to reduce the retroactive coverage window. What happens is someone goes to the hospital, and the hospital sees that they are (a) uninsured and (b) eligible for Medicaid, so they help the person get enrolled to cover the hospital’s services. This is nice for the hospital, which otherwise probably wouldn’t be able to get any reimbursement for the services rendered, but bad for the insurer, in this case, the state Medicaid agency.
Nebraska has applied for a 1115 waiver to “limit retroactive eligibility to the beginning of the month in which the individual applies for Medicaid,” which it estimates will save ~$100 million between the state and federal government.
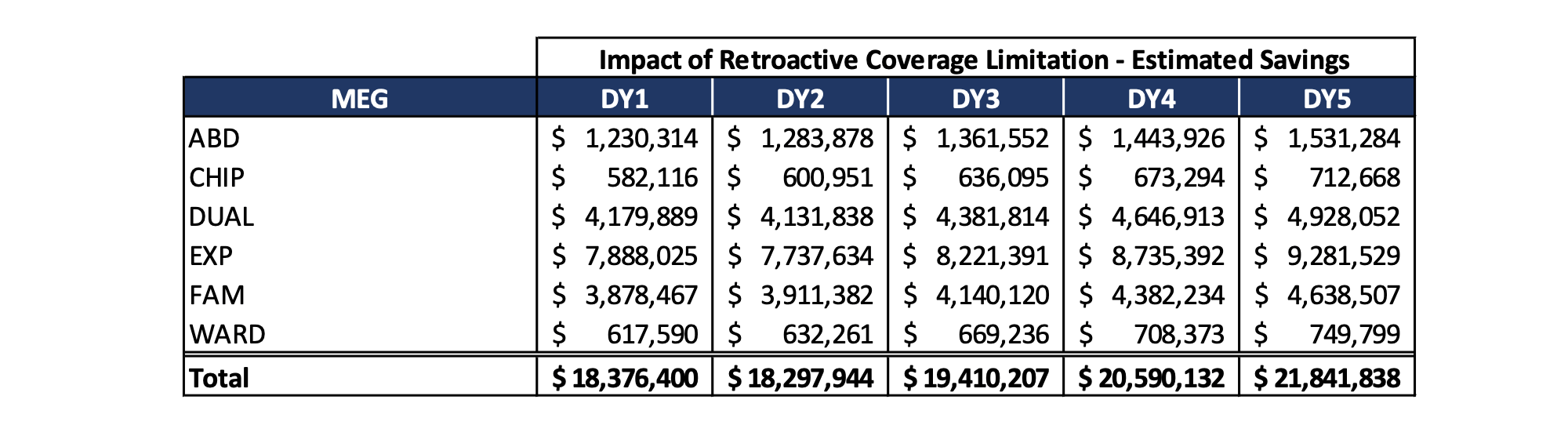
Source: Nebraska DHHS public notice
Hospitals in Nebraska are, obviously, not super pleased:
Bryan Health, which operates six hospitals in the state, estimates that its hospital system will lose about $35 million each year if retroactive coverage is set to zero, said Ashton Wyrick, senior director of government and community relations advancement.
“Really, it’s inflicting $2 worth of pain, or cost, to the hospital, for the state to save a dollar,” Wyrick said. “So it’s not necessarily a clean cut.”
That other dollar is from the federal government, for what it’s worth. It’s a tough time to manage a state budget, so you can understand why they’re looking for change in the sofa. On the other hand, it’s a tough time for some hospitals, so you can understand why they’re vociferously pushing back.
Also, from the states, Iowa is upping their provider taxes to the new OBBBA limit, North Carolina is thinking about revoking hospitals’ property and sales tax exemptions, “I would hate to see things shift toward a pack-and-ship facility”, and looking at state-level insurance filings to study variations in administrative costs and profits for health plans.
More from Health Tech Nerds
Weekly Health Tech Reads: Sutter & Allina sign LOI, Klomp's commentary at STAT, Trilliant's take on provider coding intensity, and more. Read here.
Community Brain Trust: HTN Slack updates, how North Carolina is fixing its state health plan, Allina's merger with Sutter Health, and more. Read here.
Prax Health announces nearly $10 million in financing to help NPs open up independent practices. Read here.
Health Tech Nerds Radio
The Grand Roundup: a live discussion on the healthcare news of the week. Mondays at 12pm EST / 9am PST. Join us live on LinkedIn or YouTube! This Monday, we’re looking forward to welcoming:
Toyin Ajayi, Co-Founder & CEO of Cityblock, to discuss her latest report on Medicaid + AI: cityblock.com/ai-report from 12:15-12:30pm EST.
Zack Kanter, Stedi's Founder & CEO, to discuss their $50M Series C from 12:35pm-12:50pm EST.
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.

