👋 Welcome to this Sunday’s recap of healthcare news. As we close out the first quarter of 2026, it’s clear that two trends dominating the healthcare innovation conversation this year are AI in clinical care and longevity models. Both showed up in spades this week, along with some more traditional nerdy topics like the DOJ suing health systems and provider coding intensity questions. There were twelve separate startup funding rounds announced this week, indicative of the massive opportunity investors see in AI doctors and peptide injections. Let’s dive in!
- Kevin
PS. I’ll be taking next Sunday off for Easter, but will be live with Martin for The Grand Round Up on Monday, April 6th, aka 2027 Final Notice Deadline Day, which I imagine will give us plenty to discuss 🙂
🚨 Catch The Grand Round Up LIVE, Tomorrow @ 12pm ET / 9am PT
Martin and I are quite enjoying chatting through our weekly round-ups of healthcare news on The Grand Round Up. There is so much going on in the healthcare innovation world these days that we’re finding it quite helpful to talk through it all live, in addition to this written format.
This week, we’ll be diving into topics like the great peptide debate, Martin’s reflections on the annual AHIP conference, and a dozen separate funding rounds. We’re also excited to learn from a few special guests on the show:
Toyin Ajayi, Co-Founder & CEO of Cityblock, to discuss how Cityblock is implementing AI from 12:15-12:30pm ET.
Zack Kanter, Stedi's Founder & CEO, to discuss Stedi’s $50M Series C and the future of claims clearinghouses from 12:35pm-12:50pm ET.

Top Headlines
The DOJ filed its second antitrust case against a health system in recent months, this time suing New York Presbyterian in NYC over all-or-nothing and anti-tiering / steering contract provisions. The suit is worth checking out to see the case the DOJ is making against NYP and how it thinks NYP is preventing lower-cost insurance offerings from entering the market. Perhaps it is just me, but I don’t get the sense this is a particularly strong antitrust case as I read through the combinations of NYC maps, talk of competitors offering lower prices, and the discussion of NYP’s 25% market share. It reads like an organization that knows it is the high-cost offering in the market, and is comfortable with being exactly that. The DOJ case notes that NYP conducted an internal analysis, finding that tiering would cost NYP hundreds of millions of dollars in profits each year. Certainly, anti-tiering language and all-or-nothing contracts are not helping to bring down prices for consumers, but I think there are other paths forward that are more likely to create more competition and drive down prices, if that is the primary goal given the tradeoffs at hand.
New York City Health + Hospitals is not renewing its contract with Palantir after political pushback over Palantir’s work supporting government customers, including ICE. NYC Health + Hospitals has apparently been using Palantir for revenue cycle management support, paying Palantir ~$4 million since 2023.
In the consulting world, Infosys announced the acquisition of Optimum Healthcare IT for $465 million. Optimum did $276 million in revenue in 2025, up from $107 million in 2024. Interestingly, the PE firm behind Optimum credits its growth over the past few years to an apprenticeship program bringing more people into the workforce.
OpenEvidence launched a new Coding Intelligence offering, designed to “help physicians capture every dollar they’ve earned.” Seems like an interesting strategic move for OpenEvidence, expanding beyond its core search offering into more traditional RCM functionality. I can see the logic here, but I also wonder about how the momentum translates into a competitive RCM landscape. Will be curious to see how OE reports usage here.
XO Health, an alternative plan design for employers, is expanding nationally. XO has been building an interesting value-based care network for self-insured employers, level-funded plans, and TPAs. It feels like we’ve spent the past few years talking about alternative plan designs, and we’re now at an inflection point where employers are starting to act. Going to be interesting to watch this space evolve over the next few years.
Health Management Associates announced the acquisition of HealthTech Solutions, a Medicaid-focused analytics platform.
MUSING
Should I be injecting myself with peptides?
As a kid, I grew up in an era where the only folks I was aware of who were injecting themselves with things were baseball sluggers, drug addicts, and my friend with Type 1 diabetes. Fast forward a few decades, and all of a sudden I feel like a country bumpkin for not having a longevity clinic serving as my personal peptide dealer. Check out this chart from a Sherwood article on Thursday, highlighting the massive spike in interest in peptides over the past year:
If you can’t tell from the paragraph above, I am skeptical here. Yet the other day, I was chatting with a clinician friend and asked for his opinion on peptides. I was a bit surprised when his opinion was one of measured optimism. Yes, the current grey market may be a backwater. But at the same time, there is merit behind the general idea that inhibiting inflammation leads to substantial health benefits. His general tak was that a decade from now, there’s a reasonable scenario where we look at peptides as having the same revolutionary potential as GLP-1s (itself a peptide, albeit seemingly in a different category than the grey market people refer to colloquially when discussing “peptides”).
I spent a chunk of my Monday afternoon going down the peptide rabbit hole after watching the 30-minute TBPN debate between Martin Shkreli (the pharma bro) and Max Marchione (Superpower CEO) on the merits of peptides. If you’re interested in the topic and haven’t seen it, it’s well worth your time.
Never did I think that I’d view Shkreli as a voice of reason, but alas, it is 2026, and we live in a weird world. I think Shkreli pretty clearly won the debate on its merits. Yet at the same time, I can’t help but wonder if Marchione lost the battle but will end up winning the war. Companies like Superpower and Hims seem well-positioned to pounce on this trend, particularly with looming federal deregulation. Funding announcements like eMed and VITL this week seem to signal investor expectations around a coming peptide boom. Brands like Gameday Men’s Health are quietly building up a sizeable footprint (it now has 400+ franchised clinics across the US).
The Shkreli/Marchione debate seems to sum up the current conversation around peptides quite well — the medical establishment shouts that there is no evidence peptides work. Citizen scientists respond by asking why so many people are using them if they don’t work. Both sides are making valid points, though they seem to talk past each other while generally skirting the edges of a much larger societal conversation about mistrust in institutions like the FDA that are supposed to resolve these issues for us.
The outcome here seems fairly predictable — consumers are revealing their preferences by opening their wallets to inject themselves with grey market peptides from China. Athletes seem to think they recover faster with BPC-157, so why shouldn’t I use it too? While the medical establishment yells about peptides lacking evidence, consumers don’t seem to care. As popularity grows, there will be some bad actors and bad outcomes for some individuals who don’t actually know what they’re injecting themselves with. Those bad outcomes will make for attention-grabbing headlines. Regulatory scrutiny will follow as political leaders see an easy win, and peptides will eventually settle into an established market.
As for my personal consumption of peptides, I’m comfortable being a laggard in this market, letting others experiment with grey-market compounds as that cycle plays out. That said, I’m guessing my answer to that question will change within the next five years, whether that’s an FDA-approved retatrutide or some other miracle drug coming down the pipeline.
A NUMBER TO PONDER
88%
The percentage of healthcare provider execs who think labor costs per admit will increase over the next 12 months, per a survey conducted by Health Enterprise Partners of its 150 LPs. That number seems to run counter to the various thought pieces I read about how AI will lead to an abundance of zero-cost care delivery in the near future.
The HEP survey highlighted several key industry trends and is worth perusing in its entirety, but this number stood out to me in particular. I had a chance to chat (Apple, Spotify, YouTube) with HEP Managing Partner Ezra Mehlman and Operating Partner Tom Cassels about this and other key trends in the report. Tom and Ezra shared some interesting insights into the potential for AI-fueled disruption and the fact that organizational redesign is a time-consuming process.
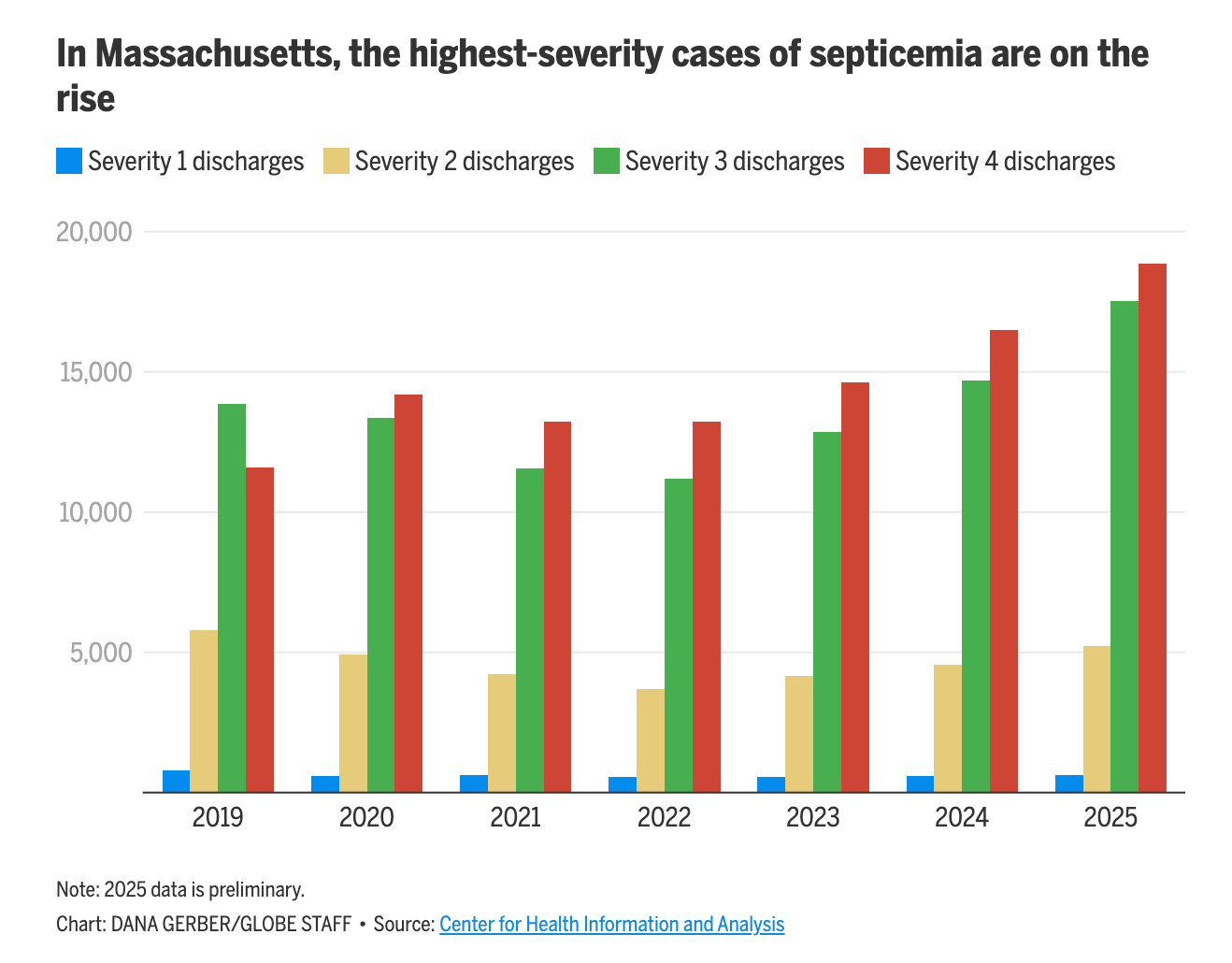
CHART OF THE WEEK
A story from the Boston Globe this week highlighted the fascinating case of sepsis in Massachusetts, which has seen a dramatic increase in high-severity discharges over the past few years, as shown in the chart below. The specter of AI-driven coding intensity is discussed as a potential reason for this increase, as AI-driven tools provide better documentation for providers.
Funding Announcements
Qualified Health, an AI platform for health systems, raised $125 million. New Enterprise Associates led the round. Qualified cites Mercy, Emory Healthcare, University of Rochester Medicine, Jefferson Health, and University of Texas System as customers using its AI platform. Qualified appears to be taking an approach akin to Palantir or Health Catalyst, deploying engineers within health systems to help them build and execute on a variety of AI opportunities.
Stedi, a claims clearinghouse, raised $50 million. Addition led the round, which comes only seven months after Stedi announced its last round. Stedi has now raised $142 million in total. It cites a 6x increase in paying customers and a 7x increase in billed transactions, processing over a billion claims and eligibility transactions annually.
Thesis Care, a startup building AI agents for clinicians, raised $45 million. Oak HC/FT led the round in Thesis, formerly known as Trovo Health. It cites thousands of providers as customers, across primary care and specialty care organizations, including US Heart and Vascular.
Doctronic, an AI model for clinical care, raised $40 million. Abstract and Lightspeed Venture Partners led the round, its third in under 12 months. Doctronic notes that it has grown 15x since it closed its Series A six months ago, generating $10+ million in annualized revenue and seeing 300,000+ weekly visitors. That math suggests it is doing ~21,000 telehealth consults per month at the moment (21k × $39 × 12 = ~$10 million), which would imply it is doing a telehealth visit for <2% of those 300k weekly visitors. Ngai Yeung shared an interesting experience using Doctronic in Endpoints this week, highlighting how AI-centric care still has a way to go, despite the promise.
Adonis, an AI-centric revenue cycle management platform, raised $40 million. Quadrille Capital led the round, with General Catalyst and Bling Capital participating, bringing Adonis’s total funding to $94 million. The press release notes Adonis saw 4x revenue growth in 2025, with net retention above 130%. Mount Sinai is quoted as a customer.
eMed, a longevity practice, raised $200 million at a $2+ billion valuation. AON Consulting led the round, an unusual name to see as a lead investor in a round like this. Then again, this whole company is a bit unusual, featuring Tom Brady as its Chief Wellness Officer. eMed notes in the press release that it feels it is the “gold standard” GLP-1 offering for employers, citing 90% patient adherence. eMed also has a D2C offering that appears ready to pounce on the longevity/peptide opportunity.
Blossom Health, an AI copilot for psychiatry practices, raised $20 million. Headline led the round. Blossom reported that hundreds of clinicians are using it to treat 10k+ patients.
Clasp, a startup that helps employers retain clinical hires via loan repayment programs, raised $20 million. Crosslink Capital and Digitalis Ventures led the round. Clasp claims to see retention rates 2.5x higher than other models. A number of large health systems are already customers — Boston Children’s Hospital, Memorial Sloan Kettering, Northwestern Medicine, Novant Health, and Ohio Health.
Dimer Health, an AI-centric post-discharge platform, raised $13.5 million. Team8 and Table Management led the round.
Prax Health, a business-in-a-box model for NP-led clinics, announced $10 million in funding across two rounds. Martin had the chance to sit down with Prax’s Co-Founder and CEO, Meghan Jewitt, to learn more about the model. It has helped 200+ NPs launch their own independent practices, tracking to 5x - 10x growth this year.
Certuma, a startup building an AI doctor, raised $10 million at a $60 million valuation. 8VC led the round.
VITL, a platform that connects compounding pharmacies with longevity clinics, raised $7.5 million. VITL reports that it currently has 630+ clinics as customers and is generating $10+ million in ARR.
Featured Jobs
Lead Director of Strategic Operations at Oak Street Health, a value-based primary care provider for seniors on Medicare Advantage. Learn more.
$160K - $200K | Remote
Director, Business Operations & Strategy at Spring Health, a mental health platform for employers and health plans. Learn more.
$177K - $221K | Hybrid (NYC)
Chief Commercial Officer at Centivo, a primary care-centered health plan. Learn more.
Remote
Director, Growth - Health Plan Partnerships at Thrive Mobile, a mobile-first engagement platform for Medicaid and Duals. Learn more.
$220K - $240K OTE | Remote
Medical Director, Health Plan at Sana Benefits, an innovative health plan for small businesses. Learn more.
$200K - $250K | Remote
Contact us to feature roles in our newsletter.
What I’m Reading
Medicaid + AI: A New Standard for Innovation by Toyin Ajayi
A good perspective on how Cityblock is approaching the implementation of AI for Medicaid populations, both in terms of theoretical principles and how it is embedding AI in the member journey.
Read more
The Future of Quality in Medicare and Medicaid: Themes from the CMS Quality Conference by Avalere Health
The Avalere team shares takeaways from the recent CMS conference on measuring quality. I find it interesting, although not entirely surprising, that the first takeaway is a shift in focus from treatment to preventive services. Annual wellness visits, nutrition, lifestyle interventions all play a key role here. Read more
Break Stuff: Ten Things the Healthcare Market Is Telling Us in 2026 by Ezra Mehlman, Jessie Gentil, Michelle Kauffman, and Culver Duquette
As referenced above, this annual HEP survey of 150+ healthcare execs provided some helpful insights into the state of AI-driven change, cost pressures on healthcare orgs, and more. Read more
Rise of the Agentic EHR by Colton Ortolf
Ortolf penned an interesting X post on the potential for an agentic EHR to supplant the “Headless EHR” concept as the EHR disruptor. It’s interesting to ponder the ‘why now” points — distribution costs going down with AI, better technology today, more SMB provider customers, and a group of incumbents facing the Innovator’s Dilemma. Read more
Doctors should be paid to keep patients healthy by Ashish Jha and Tom Tsai
An interesting series in Substack (and the Boston Globe) making a case for the path forward for value-based care — raising the stakes. Upside/downside risk, including specialty care, longer-term contracts, etc, all revolving around more accountable care. VBC nerds won’t find much new in here, but it is interesting to see how the case is made for a more general audience. Read more
High-Stakes Medicine: Rethinking Policies for the Cost and Value of Cell and Gene Therapies by Alison Sexton Ward, Elizabeth Fowler, Jeremy Shane, and Darius Lakdawalla
A helpful piece on the unique challenges that Cell and Gene Therapies present in terms of reimbursement pathways. The points raised about the financial challenges hospitals have in investing in these programs were particularly interesting, i.e. it can cost $1 million upfront to start a CGT program, with limited visibility into downstream patient flows.
Read more
HTN Content From the Week
Community Brain Trust: HTN Slack updates, how North Carolina is fixing its state health plan, Allina's merger with Sutter Health, and more. Read here.
Weekly Health Policy Briefing: A pall over AHIP, managed care by default in Medicare, and retroactive Medicaid coverage. Read here.
Health Tech Nerds Radio
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.