Sponsored by: Ursa Health
Over the last decade, Ursa Health has quietly powered some of the most expansive value-based care companies. What they built with agilon health is particularly impressive.
As a public company spanning 30+ full-risk payer contracts and 500K+ MA and ACO lives, agilon operates in an extraordinarily demanding data environment.
Ursa embedded directly with agilon's domain experts to build a financial data pipeline capable of handling this complexity and scrutiny, achieving forecasting accuracy within a fraction of a percent, extensive payer onboarding reduced by 6 months, and complete traceability from raw payer files to GL-ready outputs.
If you're thinking about VBC data infrastructure at scale, the case study is worth reading.
If you're interested in sponsoring the newsletter, let us know!
👋 Welcome to this Sunday’s recap of healthcare news. Sutter Health’s LOI to acquire Allina Health dominated the discussion early in the week, while Klomp’s commentary at a STAT summit later in the week provided some interesting signal on where Medicare is heading ahead of a much-anticipated Final Notice in a few weeks. Trilliant offered a helpful, nuanced perspective on increased coding intensity associated with AI, and I spent time reflecting on a recent conversation with North Carolina State Health Plan’s Tom Friedman. Let’s dive in!
- Kevin
TOP NEWS
Sutter and Allina announce intent to merge
California-based Sutter Health announced its intent to merge with Minnesota-based Allina Health (my last employer before starting Health Tech Nerds!), as the two parties have signed an LOI. If the merger is approved, the combined system would generate ~$25 billion in revenue annually, operating 39 hospitals across California, Minnesota, and Wisconsin.
Allina Health will retain its local market brand and leadership while becoming “Sutter Health’s Upper Midwest Division.” Sutter will invest $2 billion into Minnesota and Western Wisconsin to help improve patient access and affordability.
The nomenclature of referring to Allina as “Sutter Health’s Upper Midwest Division” seems indicative of the expansion plans for Sutter ahead, as does Sutter’s recently hired M&A leader. The Minnesotan in me may quibble with the “Upper Midwest” moniker for Allina — this is a system that now operates hospitals in California, Minnesota, and western Wisconsin… is a directional qualifier ahead of “Midwest” really necessary here?! I have to imagine the name is a tell as to Sutter’s planned strategy here. I’d be surprised if we don’t hear about more moves like this in the relatively near future.
It seems like a logical move for both leadership teams given the current state of both organizations. Sutter ambitions to enter the race of national health systems begins to materalize, while Allina secures long term stability in an uncertain healthcare environment in Minnesota. More scale generally seems to be a winning hand in healthcare. So the strategic logic here seems pretty straightforward to me, setting aside the broader questions over the societal value of cross-market mergers of health systems and whether or not there are any real synergies in a deal like this.
TOP HEADLINES
The Qualtrics/Press Ganey merger is apparently off, as banks have halted the deal due to concerns about AI in the debt markets. Back in October 2025, it was announced that Qualtrics would pay $6.75 billion to acquire Press Ganey to create a broader AI platform for customer experience.
Providence is exploring the sale of its health plan, Providence Health Plan. Providence Health Plan has 440k members across ACA, commercial Medicare, and Medicaid markets. In an email to the Lund Report, Providence’s CEO noted several factors for considering a sale, namely “rising prescription drug costs, pressure to keep prices affordable and the need to continually upgrade technology make it harder for smaller plans to keep up.” Seems like another indicator of the bleak state of regional health plans at the moment.
Verily announced $300 million in funding this week, moving Alphabet to a minority investor in the business. Series X Capital led the round, while Alphabet, UCHealth, and the University of Colorado Anschutz participated. Verily has reportedly been working for years to spin out of Alphabet, as Alphabet decided it was no longer a core business. Series X has close ties to Alphabet, after launching in 2024 to help Alphabet transition its X projects into standalone businesses.
The Seattle Times wrote a front page article about how the WISeR program has had some roll-out challenges in Washington state, articulating the real world consequences for one person who is having issues accessing medication. The article seems to get some of the factual details wrong about the WISeR model, but nonetheless seems indicative of the broader mistrust people have in prior auths at the moment, and associated political challenges for WISeR.
Chartis acquired an AI venture studio, Leap AI. Leap AI lists five businesses in its portfolio, three of which are still in stealth, in the genetics, longevity, and clinical trials spaces. It appears to be something of an acqui-hire, with Chartis leveraging Leap AI’s team to develop and deploy AI solutions for clients.
MedArrive announced that it acquired assets from Inbound Health after Inbound wound down operations of its hospital-at-home model.
VBC enabler Oasis Health Partners acquired Premier Health, a revenue cycle and practice operations platform. The press release notes that Oasis recently expanded into North Carolina via a partnership with PreferCare.
CHART OF THE WEEK
Trilliant’s exploration of hospital coding intensity
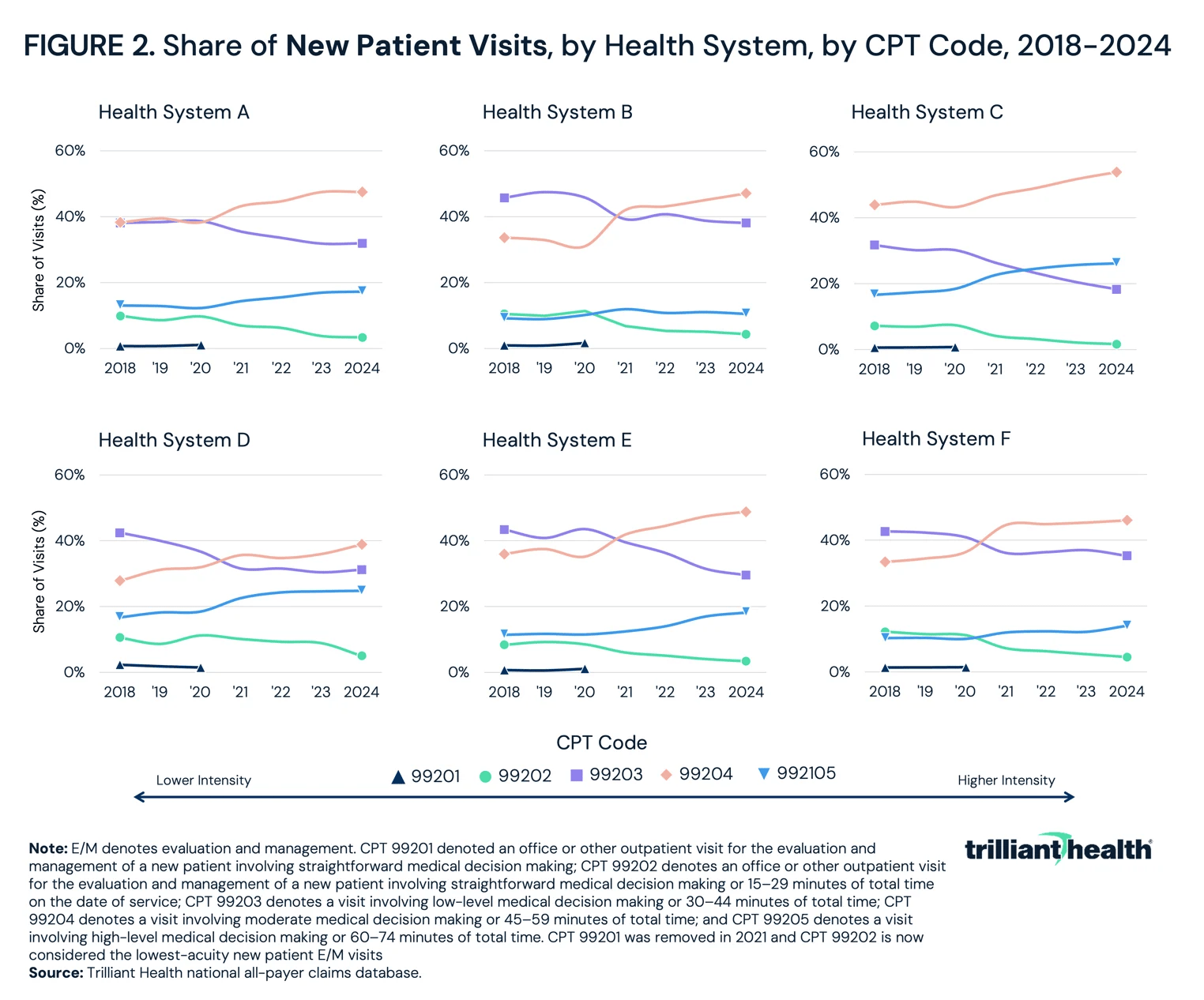
The Trilliant team shared a thoughtful perspective on the role of AI in increasing coding intensity in health systems. It explored data for six health systems that have adopted AI scribes and found a consistent upward trend in intensity of outpatient E/M visits across new and established patients. The article does a nice job thinking through the various levers that might be driving this. Check out the chart below, which highlights the steady increase in coding intensity for New Patient Visits across the various health systems.
MY MUSING
A reflection on building trust in healthcare innovation
Last week I had the chance to record a podcast episode with the North Carolina State Health Plan’s Tom Friedman, discussing the efforts underway to turn around the plan. North Carolina has always served as a fascinating test bed for healthcare innovation in this country, in part due to the active role the State Health Plan (SHP) has played.
Friedman and others penned a Health Affairs Forefront article late last year outlining their effort to turn around the plan, which covers ~750,000 lives in North Carolina and was projected to be at a ~$1 billion deficit by the end of 2027. A number of aspects of this effort fascinate me, including the decision to unwind the Clear Pricing Project, a prior initiative aimed at driving price transparency and ultimately reducing costs in the market via a reference-based pricing model. The Clear Pricing Project was a great case study in how efforts to drive cost savings can have the opposite of their intended effect, increasing healthcare costs in the state (providers who were historically paid below the RBP rate chose to participate; those who weren’t didn’t need to participate, thus increasing costs).
One of the key efforts Friedman and the SHP are now rolling out is becoming more of an active purchaser of surgical care, and specifically, offering zero-cost bundles for specific surgery types in partnership with Lantern (which just announced a funding round this week). As part of that, the SHP is attempting to influence its enrollees’ behavior to drive volume to lower-cost providers, and Novant Health joined the effort as well.
One of the topics Tom and I discussed was the need to build trust with SHP employees when rolling out these changes, particularly after coming in and raising premiums for those employees as part of fixing the deficit for the SHP. He made the point that payers haven’t historically been particularly good at building trust, and that building trust is key as the SHP rolls out programs like these. It’s a fascinating framing as a critical ingredient in driving successful uptake of innovation initiatives. This concept of building trust seems to come up in most conversations I have these days, and feels like a critical element of any healthcare effort.
A QUOTE TO PONDER
Medicare Director Chris Klomp spoke at STAT’s Breakthrough Summit East this week. Some of Klomp’s commentary was picked up by Bloomberg on Thursday, suggesting that the Medicare Advantage program is not sufficiently managing costs.
It is fascinating to juxtapose that headline with this quote from his interview with STAT’s Mario Aguilar, also at that event, about potentially enrolling Medicare beneficiaries into MA by default:
Klomp: CMS has a stated goal and this precedes the Trump administration, the Biden admission and beyond that every beneficiary, being an accountable relationship. Why do we care about that? We just talked about it because accountable relationships lead to higher quality measures, a better clinical experience, better clinical performance. It's healthier beneficiaries, healthier patients. And so could we see a default selection into an accountable relationship, which could be an ACO through the Medicare Shared Savings Program or a derivative or successor CMMI model from the Center for Medicare and Medicaid Innovation led by Director Sutton? Yes. Could it be through a Medicare Advantage enrollment? Yes.
Would either of those, in my view, be superior to a default enrollment into a fee-for-service arrangement where there's not this long-term secular relationship between the beneficiary, the patient and their provider? Yes. Why? Because we see healthier beneficiaries. That's a good thing.
Aguilar: Is that something you think we'll see in this administration?
Klomp: It's something we're considering.
I think if you stitch together the various statements Klomp has been making over the past several months, there’s an interesting common thread coming from CMS at the moment. This idea of encouraging long-term, accountable relationships with enrollees seems central to the broader narrative at hand, which I think most would agree seems like a good thing.
So if I think about that relationship as the central tenet of what CMS is trying to accomplish, while simultaneously ensuring that programs like Medicare Advantage are good stewards of taxpayer resources, the commentary all seems to fit together nicely.
Funding Announcements
Latent, an AI platform for specialty medicine approvals, raised $80 million at a $600 million valuation. Spark Capital and Transformation Capital. The press release notes that Latent has impressive traction with health systems — Latent reports 45 health systems as customers, including half of the top 20 systems in the country. Ochsner Health reported 30% YoY growth in its specialty pharmacy business working with Latent.
Turquoise Health, a price transparency platform, raised $40 million. Oak HC/FT led the round, bringing total capital raised to almost $100 million. Turquoise has ambitions as a contracting platform for healthcare organizations. The company reports having 280+ customers, including leading health systems, payers, pharma companies, and insurance brokers.
Lantern, a surgical care network for employers, raised $30 million. Morgan Health and Echo Health Ventures led the round. Check out the interview with North Carolina State Health Plan’s Tom Friedman for an example of how Lantern is rolling out with that client.
Conduit Health, a DME platform, raised $17 million. Drive Capital led the round.
Nadia Care, a maternal care model, raised $12 million. Valtruis led the round along with an unnamed national payer. Nadia, formerly known as Cayaba Care, has been working with regional Medicaid plans in DC, Maryland, and Tennessee.
What I’m Reading
CMS Proposes Its Best NBPP Yet by Brian Blase
Blase calls this the best Notice of Benefit and Payment Parameters that he’s seen. noting the expanding options, increased competition, and payment integrity reforms, among other things. Read more
What’s Worse than a Ghost Network Plan? A No-Network Plan by Sabrina Corlette, Jason Levitis, and Lindsey Murtagh
A group from Georgetown’s CHIR critiques the NBPP’s encouragement of non-network plans in the ACA market, arguing that it ignores the realities of healthcare in the country today. Read more
Doximity Study Finds Physicians Rapidly Adopting AI, But Accuracy Concerns Persist
Doximity shared findings from a study it conducted on physician adoption of AI. Nothing groundbreaking, but good data points on how physicians are using AI in practice. Read more
The Peptide Boom Is Getting Out of Hand by Nicholas Florko
I must admit, I don’t pay too much attention to peptides. This week, they piqued my attention. Between this article in The Atlantic and Martin Shkreli’s X post, it will be interesting to see how mainstream this grey-market peptide craze conversation becomes. Read more
HTN Content
Community Brain Trust: Developments in fertility care delivery, Governor Walz's Medicaid overhaul proposal, evaluating AI tools for mental health, and more. Read here.
Weekly Health Policy Briefing: MedPAC recommendations, state-directed payments, and the ESRD bundled payment. Read here.
Increasing the number of safe days at home for children with special health care needs | Taylor Beery, Imagine Pediatrics. Read here.
Health Tech Nerds Radio
Featured Jobs
Senior Director of Data Science, Clinical Performance at Pearl Health, a primary care physician enablement platform. Learn more.
$210K - $250K | Remote (or Seattle, NYC, Boston)
Customer Success Manager at Parakeet Health, AI voice agents automating practice operations. Learn more.
$110K - $150K | In-office (SF)
Finance Associate at Cartwheel Care, provider of pediatric and adolescent behavioral health services via partnerships with school districts. Learn more.
$90K - $140K | Remote
Program Manager Clinical Innovation Business Insights at Ascension, a nonprofit health system operating 90+ hospitals across 17 states and DC. Learn more.
$82K - $115K | Remote
RCM Strategy and Operations Manager at Alpaca Health, building a practice-in-a-box for autism care providers to launch independent practices. Learn more.
$80K - $120K | In-office (NYC)
Contact us to feature roles in our newsletter.
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.