Washington, D.C.
People like to complain about MedPAC, the nonpartisan, independent agency that’s part of the legislative branch and advises Congress on the Medicare program. I think these complaints are generally a bit motivated, but it’s certainly the case that MedPAC has something of a house view, and that view is articulated in excruciating detail in its semiannual reports to Congress, the latest of which was released last week.
For those of you who haven’t had the chance to peruse the nearly 600-page document, this house view is:
Health care spending, generally, and Medicare spending specifically has been growing faster than Gross Domestic Product
Medicare spending growth is driven by a combination of factors, including programmatic changes to Part D, rising enrollment, and growth in volume and intensity of items and services
To finance the rising spending, the country is increasingly relying on federal income taxes, increasing beneficiary premiums, and issuing debt.
MedPAC also highlights provider consolidation and health care staffing shortages as ancillary issues that exacerbate these problems, but its main focus, as required by law, is an assessment of the adequacy of Medicare Fee-for-Service payments and a recommendation on updating payments.
For Hospital inpatient and outpatient services in 2027, MedPAC recommends
no change to what’s currently projected to be a ~2% increase
adopting a MedPAC proposed formula to calculate uncompensated and disproportionate care payments to hospitals called the Medicare Safety Net Index (MSNI), and increasing the MSNI pool by $1 billion
expansion of site-neutral payment policies
For the Physician Fee Schedule, an increase to physician and other health professional services by an additional 0.5% more than current projections, which, after the temporary 2.5% increase expires, translates to a payment reduction of 1.2% or 1.7% based on the payment program.
For End Stage Renal Disease, no update to the 2026 base rate, rather than the 1.6% increase projected under current law
For Skilled Nursing Facilities, a reduction of 4% from the 2026 base rate
For Home Health Care, a 7% reduction from the 2026 base rate
For Inpatient Rehabilitation Facilities, a 7% reduction from the 2026 rates
For Hospice, no update to the 2026 base rate instead of the 1.6% increase projected under current law
MedPAC also gets instructions from Congress to write various status reports on things like Ambulatory Surgery Centers, for instance, which MedPAC thinks should be required to submit cost data in the same way hospitals are required to, and the Dual-Eligibles program, for which MedPAC has concerns W/R/T plan integration.
But MedPAC connoisseurs will flip immediately to the Medicare Advantage status report first because this is where its house view causes the most consternation. It’s where you get charts like these that assert that while it’s improving, Medicare Advantage payments are higher relative to Fee For Service:
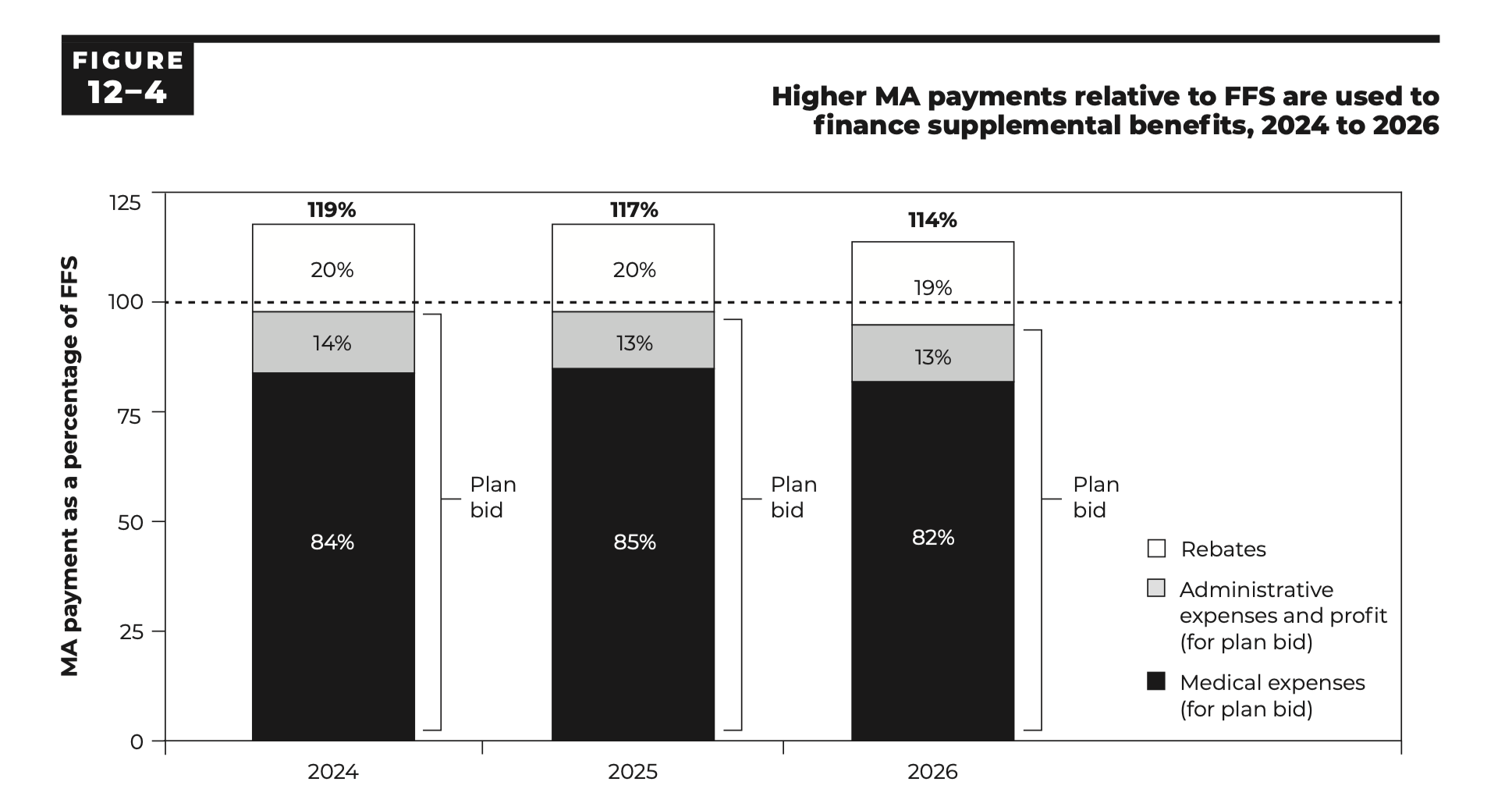
And those higher payments are driven by coding and favorable selection:

MedPAC’s recommendations aren’t law, and these recommendations, criticisms, and comments are free to be ignored by Congress and CMS. There are contentious methodological disagreements among MedPAC, CMS, and industry groups in the pages of Health Affairs and in the Wall Street Journal's letters to the editor section. But if you’re interested in health care policy and financing, these semiannual reports and other releases are as valuable as public goods as our national parks are to outdoorsy types.
Also in Washington, D.C., dark money groups try to influence the 2027 final rate notice, The Make America Healthy Again: Enhancing Lifestyle and Evaluating Value-based Approaches Through Evidence (MAHA: ELEVATE) Model notice of funding opportunity is live, and Congress is back in town and held hearings this week on the NIH; the role of CMS in combatting waste, fraud, and abuse; providers and hospitals and their role in the affordability crisis, and improving kidney health through better prevention and treatment.
State Capitols
A nice thing, if you’re a state with a balanced budget requirement in your state constitution and residents who don’t like tax increases, is to figure out some way to get the federal government to contribute.
For what ended up being a pretty long period of time, there was something of a cottage industry for pulling this off for Medicaid between provider taxes and state-directed payment programs. We’re approaching the end of that era with the implementation of the One Big Beautiful Bill Act, which is making the artisanal statistics and creative payment formulas a lot less lucrative.
But a CMS interpretation of some H.R.1 language is giving states the opportunity for one last hurrah:
While the law allows grandfathering for plans that start within 180 days of enactment, CMS instead chose to interpret this as 180 “business days.” This is a meaningful distinction, as it grandfathers through March 27, 2026 instead of December 31, 2025 – allowing new and increased payments at the beginning of the year (as many are) to pay far above Medicare rates, so long as applications were submitted before the law was enacted on July 4, 2025.
This seemingly small change to the grandfathering rule comes with costly repercussions. The law currently allows states to pay SDPs up to the average commercial rate. Given the large difference between commercial and Medicare rates and slow phase-down rate for SDPs, allowing large payments to be initiated this year will increase federal costs for years to come. For example, Florida’s average commercial rate is 3.5 times Medicare rates. If CMS approves SDPs at that rate, it could take up to 10 years to phase down, depending on how CMS interprets the phase-down methodology.
The basic idea behind a State Directed Payment is that a state can use it to pay higher reimbursement rates for Medicaid, which incentivizes more providers to accept Medicaid. It’s been really effective! Perhaps too effective.
H.R.1 takes the punch bowl away from the party, but dedicated state Medicaid agency staffers in Illinois and Texas are making sure they get a few more cups worth on the way out.
Also, from the states, Connecticut is hiring a PACE Director, Colorado fiscal estimates were a little off for the Covering All Coloradans program, Sutter Health and Allina to merge, fraud watch, and states eagerly await work requirements guidance from CMS.
Puts & takes
I’m quite comfortable with the percentage of GDP we spend on health care in this country. In the same way that the very affluent in our society seem to be spending an increasing share of their accumulated wealth on “longevity,” I think it’s pretty sensible that a rich country like ours should be a little more indulgent and a little less price sensitive when it comes to the health of its citizens1.
This is a pretty lonely position at the moment. The general consensus is that we should spend less, and the interest in policy circles in D.C. right now is in how to accomplish this. One approach that’s been pretty successful, if you define success as how deflationary it has been, is the ESRD bundled payment program, which was introduced in the early 2010s.
The mechanics are pretty simple: dialysis providers get a bundled rate per treatment, which has to be stretched to cover all the costs associated with treatment. Just as important as the bundle mechanics, however, are the annual adjustments made to the bundle. Prices tend to rise, so the bundle gets increased most years, but importantly, the bundle has increased at a lower rate than the prices, which has led to dialysis providers ending up getting less in the way of reimbursement in real dollar terms.
For illustrative purposes, this chart looks at the per-patient-per-year spending for the ESRD program, Medicare, and, though it’s a bit apples-to-oranges, the Employer Sponsored Insurance family premium per enrollee to give you a sense of how the bundled payment has moved in comparison to commercial insurance.
This first chart uses the General Consumer Price Index as the deflator; i.e., we’re saying that compared to how the prices of goods and services generally increased between 2010 and 2020, the per-patient spending on ESRD decreased by about 8%.
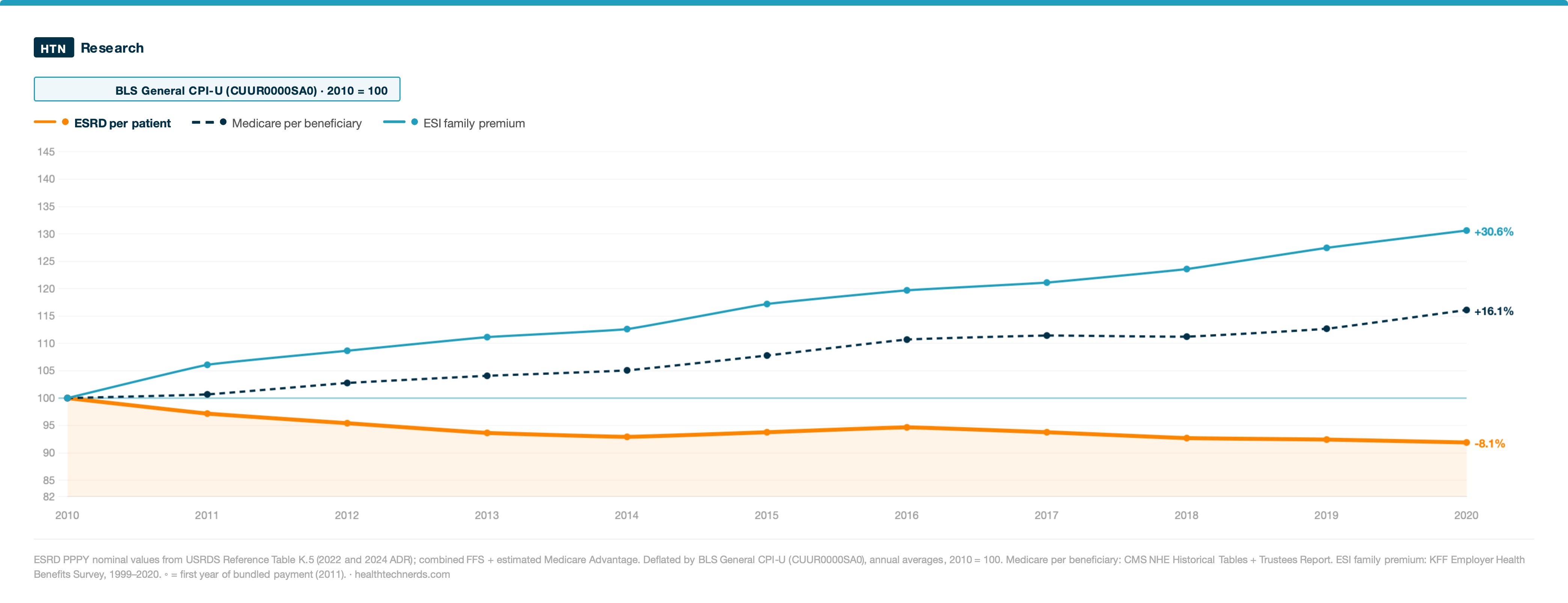
This second chart uses Medical Care Services CPI, technically CUUR0000SAM, i.e. the price increases specific to health care. Using this deflator, we’re looking at a 15% decrease.

If the only thing you care about is prices, this is an incredible feat! While spending was increasing everywhere else in healthcare, the ESRD bundled payment program is spending less money, in real terms, than it did a decade ago.
Of course, there are people who care about things other than prices. Kidney care financing expert Tim Fitzpatrick talked about the double-edged sword of the bundled rate when we spoke last week, and University of Washington professor Suzanne Watnick, MD, FASN, wrote about innovation stagnation in kidney care in Health Affairs Forefront, which pointed to the consolidation and lack of research investment downstream from the bundled rates.
A different way to think through the trade-offs of lower prices is to imagine a world where the US health care system more closely resembles today's dialysis centers. Care is delivered by highly efficient, highly levered, vertically integrated corporate operators in strip malls and office buildings. Innovation is stagnant because the system pays for what's in the bundle, and what’s in the bundle is what gets delivered and nothing more. I don’t think this is particularly dystopian or anything. The system works for ESRD patients, DaVita shareholders, and the taxpayer-financed Medicare program. But it also feels like we could do better, which might involve spending some more money.
More from Health Tech Nerds
Weekly Health Tech Reads, 3/15/26. Read here.
Increasing the number of safe days at home for children with special health care needs with Taylor Beery, Imagine Pediatrics. Read here.
Community Brain Trust: Developments in fertility care delivery, Governor Walz's Medicaid overhaul proposal, evaluating AI tools for mental health, and more. Read here.
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.
1 I do have some thoughts on (1) how we could better allocate all those dollars we’re spending and (2) how we very obviously need to raise taxes on basically everyone to finance our current rates of health care spending, but these are conversations for another time.

