
👋 Welcome to this Sunday’s recap of healthcare news. UHS’s acquisition of Talkspace and the latest twist in the Hims / Novo saga were the top topics of convo this week. While Q4 earnings season is over, a handful of banks hosted conferences this week, with some interesting updates from public payers and providers. This week also included some fascinating AI funding rounds from companies with thoughtful use cases. As I watch the snow pile up outside my window in Minnesota this AM, I spent some time musing about my 1L Torts class years ago and its implications on liability in an AI-centric world. What could be more fun than that? Let’s dive in!
- Kevin
BIG NEWS
UHS acquires Talkspace for ~$835 million in latest behavioral health merger
Hospital operator United Health Services announced it is acquiring virtual behavioral health provider Talkspace for $5.25 per share, or ~$835 million, in order to grow its outpatient behavioral health business. UHS noted in a call Monday morning that its growth in outpatient behavioral health has been slower than it would have liked, so it was pursuing partnership conversations in the space. When Talkspace initiated a sale process, UHS viewed it as an excellent fit and jumped. It’s going to be fascinating to see the merger timeline here when that is filed and how competitive the process was.
UHS highlighted a few key pieces of Talkspace’s business that drove the interest. First, the virtual offering provides a step-down for UHS, and vice versa. Talkspace’s membership also skews younger and more commercial insurance. And perhaps most importantly, UHS gains Talkspace’s network of 6,000 therapists. It is interesting to note that those therapists are not employed by Talkspace, but UHS views this as an opportunity to build deeper relationships with therapists who might own their own practices.
As I think about M&A in both the mental health market and care delivery more generally, organizations with best-in-class provider groups seem particularly well-positioned strategically. Now, whether a contracted group of virtual therapists meets the bar for best-in-class seems like a slightly different question. Clearly, UHS thinks highly of that asset here. The takeaway remains: If I’m a digital health entrepreneur, I’m investing organizational resources to build a best-in-class clinical team and finding profitable payor contracts to support them.
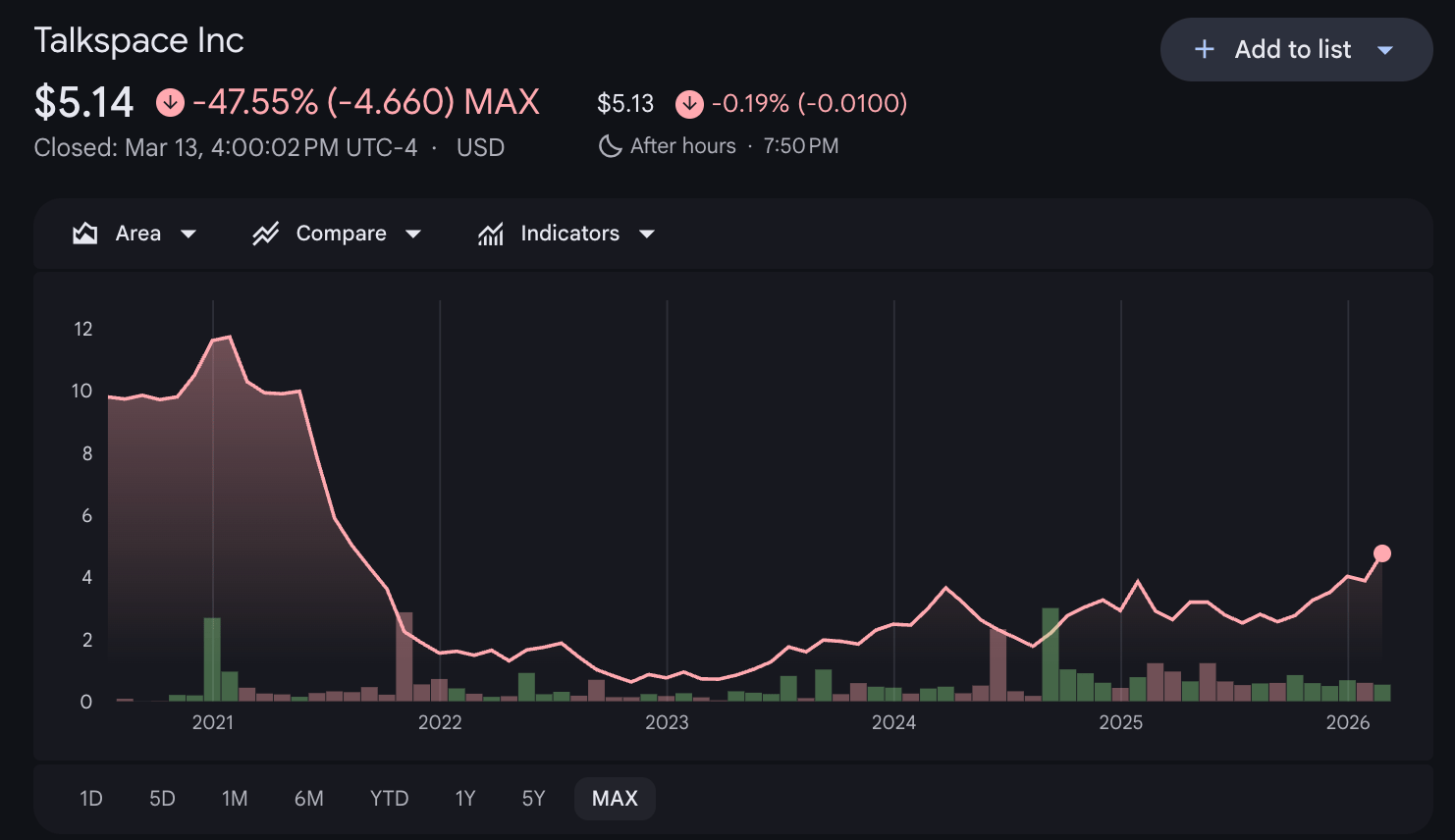
Talkspace was projecting 2026 revenue of ~$280 million and adjusted EBITDA of ~$32 million, implying a forward revenue multiple of 3x and EBITDA multiple of 26x. Seems like a pretty good outcome for a business that was trading at less than cash value a couple of years ago. The stock chart below highlights the challenging journey Talkspace has been on since it went public via a SPAC in June 2021. The transition from a D2C provider to a healthcare business has proved challenging, though if you bought into Talkspace after the COVID-bubble valuation reset, it has generated a reasonable return. Seems indicative of so many stories in healthcare innovation over the past few years.
Other Top Headlines
Hims and Novo officially announced a new partnership on Monday. Hims agreed not to advertise compounded GLP-1 offerings, although the language in the press release notes that patients still can access them via the platform. Novo agreed to drop its lawsuit against Hims as part of this process. This is the latest chapter in a long, drawn-out journey for these two companies that originally announced a partnership almost a year ago, which lasted only a few weeks before Novo backed out and accused Hims of deceptive marketing and illegal mass compounding. The stock swings tell the story here: Hims stock is up ~52% on Novo’s about-face here, while Novo is down 23% over the past month. While Hims still has a number of critics (its short interest is currently hovering around 41%), as the author of the Hunterbrook short report on Hims put it on X this week, Hims appears to have “wiped the floor” with Novo here. Certainly seems to indicate the power of the Hims brand and distribution capability.
Elsevier acquires patient engagement platform Mytonomy. Mytonomy’s video-based platform will strengthen Elsevier’s broader content capabilities. The press release notes that clinicians are worried about misinformation moving forward, as most patients self-diagnose themselves online in the next 2-3 years. Mytonomy’s SaaS offering is currently used at 70+ hospitals and 200+ clinics.
MedPAC’s very long annual report to Congress came out Thursday night, which, among other things, suggested that the $615 billion the federal government will pay to Medicare Advantage plans in 2026 is roughly 14% higher than it would pay if those members were in fee-for-service Medicare. The primary driver of this is perceived favorable selection, with coding a secondary driver.
MUSC acquired Palmetto Primary Care Physicians, the largest independent provider group in South Carolina, for $111 million. PPCP, which will become a non-profit under the MUSC umbrella, has 31 physicians and 95 APPs across 40 practices. PPCP had previously announced a partnership with agilon in 2022, which noted it was the first primary care group in South Carolina to move to a full-risk VBC model in South Carolina. PPCP noted that the MUSC acquisition will ensure long-term stability and deliver stronger value-based care, which perhaps seems like a nod to v28-induced financial concerns with a global cap model.
Remote monitoring platform Cadence confirmed it plans to participate in the CMMI ACCESS model, making it one of the first companies to publicly announce its intent to participate. It is interesting to see the quotes about how Cadence intends to use the model to embrace an AI evolution of the business. It’ll move from traditional RPM codes, where there is a monthly human interaction, to this model, where more of the work will be done by AI agents.
Aetna has agreed to pay $117.7 million to resolve upcoding allegations in the Medicare Advantage program. The settlement involves two separate issues, with $106 million tied to a chart review program it operated in 2015 and $11.5 million tied to an issue with codes for morbid obesity between 2018 and 2013. A whistleblower will receive $2 million as part of the second issue.
BV Investment Partners acquires a majority stake in Moxe Health, a clinical data exchange platform.
A Number to Ponder
~700
The number of clinicians delivering care via Devoted Health’s Medical Group, as Devoted has apparently quietly built a sizable medical group. A Devoted job posting for a primary care ops role noted that those nearly 700 clinicians delivered 200,000+ encounters last year, which, if you do the math, equates to roughly 1.1 encounters per workday. Perusing LinkedIn jobs, it appears that many of these roles are full-time NPs. Devoted also noted in the job posting that it has 5,000 AI agents automating workflows.
If AI is making care delivery more efficient, it does not appear to be showing up in Devoted’s data yet. The theme of “AI is everywhere but the jobs data” rears its head again.
Yet if you look across Devoted Health’s 47 open job postings, they paint a really interesting picture for Devoted. As I skim the jobs, it reads like a care delivery organization more than a payer, a theme we’ve also heard from other Medicare Advantage upstarts recently (c.f. Alignment, Clover). Devoted’s roles appear to indicate that it is heading down the path of building virtual centers of excellence to provide care for members with common chronic conditions (which feels a lot like… a private-payer version of an ACCESS-like concept?).
It makes me wonder if, at some point in the near future, we’re not talking about Devoted as an MA plan, but rather a virtual health system that contracts across all lines of business. A virtual national Kaiser of sorts?
A MUSING
Judge Cardozo, red teams, and a new AI regulatory framework
In news that probably won’t surprise many regular readers, I was one of the few crazies who quite enjoyed my 1L year of law school. I wasn’t a particularly great law school student, but some lessons nonetheless managed to stick with me, or at least that’s what I tell myself. Allow me to take a trip down memory lane for a second, going back to Torts.
One of the most interesting series of cases in Torts related to product liability in the early 1900s. Judge Benjamin Cardozo, whose name now hangs on buildings all over the country, featured prominently in this narrative for his role in reshaping product liability law after the Industrial Revolution.
The Industrial Revolution brought significant societal change. One particularly vexing issue in the legal world centered on product liability. For the first time in history, companies could mass-produce and distribute products. This fundamentally changed the relationship between a buyer and a seller and caused chaos for decades as courts wrangled over how to assign liability when unforeseen circumstances after a sale gave rise to a tort. There were a series of court cases about topics like the explosion of a steam boiler, a defective balance wheel for a circular saw, and a falsely labeled bottle of poison that all struggled with this issue. Yes, that is what people discuss in law school. The traditional legal framework was that two parties needed to have a contract directly with each other, “privity of contract”, for there to be negligence. Historically, that framework made sense because there weren’t mass market goods — buyers and sellers had a very different relationship.
Then along came Cardozo, who in 1916 upended this framework in the landmark case MacPherson v. Buick, which involved Buick negligently selling a defective car via a car dealer. The purchaser, Mr. MacPherson, was subsequently injured by said car. Buick argued it was not liable to Mr. MacPherson because it had a contract only with the dealer, not with him. This was the old world of “privity of contract” liability. Cardozo did away with that, holding Buick liable to MacPherson for negligently making its product, despite the two not having a direct contract. This ruling from a century ago still informs product liability today.
One of the takeaways from the class was that while Cardozo was certainly a smart guy and is now viewed as a giant in the legal field, he also benefited from coming along at the right time, after decades of prior legal decisions had made it clear that the current framework was wrong. Put differently, he needed to see the court cases from previous decades that were decided in odd ways to develop a new standard. Innovation is always ahead of regulation in that way, and it needs to be, to point out the flaws in existing frameworks.
I’ve been thinking about that lesson a lot over the past few weeks as we enter the AI revolution era. Responding to the changes this era will bring will require new regulatory and legal frameworks that account for today's evolving technologies. One of the most interesting framework shifts, in my opinion, centers on the changing relationship between a patient and a provider, specifically the interplay between humans and AI in providing clinical care.
I’ve been fascinated by the recent reactions to how an AI security firm exposed security vulnerabilities in Doctronic’s AI chatbot. If nothing else, Mindgard’s report is a fascinating dive into the workings of an AI chatbot. The bit about getting the Doctronic AI to respond in Creole was amusing, while the part about generating misleading SOAP notes was concerning. Perhaps the most concerning part was Doctronic support’s apparent lack of response to it all after Mindgard made the issue known.
But I find the consternation over the report I’ve seen on social media a bit overblown, on two fronts:
A user would have to prompt Doctronic with this information to respond in this way. Perhaps it's just me, but going back to the liability conversation, I’m not sure it’s on Doctronic when you knowingly hack its source code and supply fake official public documents to intentionally misuse the system.
While Doctronic’s pilot with the state of Utah is well-documented, my understanding is that the public-facing chatbot is “Doctronic 1.0,” and the version used in Utah is “Doctronic 2.0.” I’m not sure of the specifics, but it appears there are significantly more safeguards in place in Utah than in the public-facing chat that Mindgard accessed, as one might expect. That seems like a good thing, and gives me more confidence in Doctronic rolling this out.
Stepping back from the Doctronic example, it all highlights that we are entering a new era, one where the regulatory and legal frameworks still need to be sorted out. We’ve seen Prenuvo sued in the last few months for misinterpreting a scan. We’ve seen providers suggesting that CMMI’s ACCESS model will shift liability onto PCPs in exchange for a small payment. We’ve seen states start to propose paths forward here, with New York proposing a law that would hold AI companies liable for their chatbots. Just last week, Chris Klomp mentioned at the Better Medicare Alliance Executive Summit how we need a new regulatory framework for healthcare to see the positive impacts of AI. I very much agree with that. I’m just not sure what it looks like yet personally.
What I am more sure of is that more will need to go wrong over the coming years before we reach a coherent new regulatory standard that effectively articulates what liability will look like in this AI-centric world when things do go wrong. That is going to be a really hard process to go through in modern times, and it seems inevitable that some villains will be created along the way, fairly or not. But at some point, the AI-revolution equivalent of Benjamin Cardozo will come along and redefine the rules, setting us on a better path in the future.
Until then, we’re going to be in a messy period where things do go wrong from time to time, and we will all need to grapple with the consequences. This era of AI innovation will almost certainly entail the unfortunate reality that modern-day versions of Mr. MacPherson will be harmed. Yet suggesting we halt progress here because of concerns over “doing no harm” seems to ignore the fact that, despite best intentions, the medical system indeed still sometimes harms people today. If my Torts class taught me anything, it’s that it is the inevitable path forward for us all, and ultimately, that will be a good thing societally.
Public Markets Updates
While the Q4 2025 earnings season is now in the rearview mirror, there were a number of health plan and health system presentations at bank conferences this week. Here’s a quick sound bite from each of the sessions I found myself tracking along with this week, broken down by plans / providers:
Plans:
Alignment noted that it expects a solid opportunity to grow in 2027 as large plans continue to prioritize margin, and the smaller private / not-for-profit plans that grew significantly in 2026 are going to experience issues. On the topic of Advance Notice, the conversation referenced a recent Wakely report suggesting that some plans could see a 6% rate cut from de-linking chart reviews. Kao also noted the miscalculation on skin substitutes, which could be a 1.5% to 2% lift for rates in the final notice, before noting that he expects the final notice could get to 4% on the whole, above the 2% to 3% most are expecting.
Centene is seeing its ACA membership decline tracking in line with expectations, with its ACA book down 40% over the year, while the industry is closer to the high-teens to mid-30% range.
Clover Health again touted the strength of its AI-forward model, noting that while the industry is expecting a 2% to 5% increase in the final rate notice. It said at one point that it would “welcome… an almost flat rate increase because it will show the strength of our model.” As Martin and I have been discussing recently, the game theory here is fascinating.
CVS's discussion was pretty straightforward; it spent a decent chunk of time discussing its new consumer-facing AI initiative, Health 100. I still do not understand it, but the organization seems excited about it.
Elevance noted that it viewed its recent issue with CMS not as a data transmission issue but rather as a policy issue regarding risk adjustment data from pre-2023. On the ACA front, early member effectuation data suggest it is tracking with previous years, which would imply less attrition than the industry has been expecting.
Humana stated more clearly that it will need to adjust benefits to respond to the overall rate environment in MA moving forward, which will put Humana’s LTV thesis to the test. Humana outlined that one of the key financial drivers of LTV, in addition to managing medical costs, is the reduction in member acquisition costs going from year 1 to year 2. Acquisition costs decrease from $1,000+ per new member in year 1 to around $500 in year 2. My rough math on that implies it’s ~4% in margin improvement on that number alone.
UHG noted that it is exiting VBC contracts in OptumHealth that range from a -2% margin to up to -11% margin, and rightsizing the VBC membership will turn into a tailwind as it moves into 2027 and attempts to move back toward its target margin.
Providers:
HCA spent time discussing its $600 to $900 million ACA headwind in 2026 from disenrollments and noted that 2026 is coming in at the lower end of expectations. It also noted that there could be more disenrollments in 2027 as families work through the financial impact of ACA plans without subsidies.
Tenet continues to position itself quite well overall. There was an interesting Q&A about site-neutral payments and how ASCs will continue to differentiate if hospital outpatient reimbursement is the same. Tenet does not seem particularly worried about site-neutral payments coming to reality in a meaningful way, i.e., for complex surgical cases.
agilon again discussed its high-cost members ($1+ million in medical expense) in 2025 after revising its full-year trend assumption from 5% to 6.5%. agilon noted that it usually expects to have 2 to 3 of these members per year, but they ended up having 2 or 3 in one quarter, with one of those patients.
Surgery Partners discussed three markets that have driven its recent underperformance, including one in which it captured an unexpected share of Medicare Advantage business as other providers went out of network. This left it as the lone independent surgical facility available to patients, leading to an influx of MA members at the expense of commercial volume.
Teladoc continues to execute on its turnaround, expressing optimism about the growth trajectory of BetterHelp’s insurance business, which it believes will eventually offset declines in the consumer-facing business. BetterHelp noted that 80% of members drop the cash-pay model because of cost, which insurance should help it tap into. Teladoc expects US-focused M&A to continue.
Featured Jobs
Customer Success Manager at Parakeet Health, an AI patient engagement platform. Learn more.
$110K - $150K | In-office (SF)
Head of Marketing at Sword Health, an AI-enabled virtual MSK and cardiometabolic care provider. Learn more.
$400K - $630K | Remote (US)
Vice President, Finance at Waymark, a community health worker model for Medicaid patients. Learn more.
$140K - $259K | Remote
Chief Growth Officer at Equality Health, a value-based care model for Medicaid. Learn more.
Sr. Manager, Partnerships Strategy and Operations at Oshi Health, a virtual gastrointestinal care provider. Learn more.
$140K - $170K | Hybrid (NYC)
Contact us to feature roles in our newsletter.
Funding Announcements
AMI Labs, a “world model” for AI with deep ties to AI scribe startup Nabla, raised $1.03 billion in Seed funding at a $3.5 billion pre-money valuation. Nabla is noted as the first partner for AMI, after the two parties announced an exclusive partnership in December. AMI was founded by Nabla founding investor / advisor Yann LeCun, and Nabla’s now-former CEO Alex LeBrun has stepped into the role of CEO at AMI.
Nitra, an AI platform helping practices manage finances, raised a $72 million Series B. It announced $187 million in total financing across the Series B, a $22 million Series A, $20 million in venture debt, and a $95 million warehouse facility. Nitra noted it grew to $33 million in revenue in 2025, up from $4 million in 2024, and expects to generate $150 million of “annualized revenue” in 2026. It is working with 700 clinics today and expects to process $4 billion in transaction volume in 2026 for its customers, which appear to be specialty practices in the ophthalmology, dermatology, urology, and medspa markets.
Translucent, an AI agent for hospital finance departments, raised $27 million. Google Ventures led the round, which comes less than a year after it raised Seed funding in August 2025. Translucent is providing customers, including Northwestern Medicine and Duly Health and Care, with better financial data to help hospitals improve margins. Seems like a very cool, targeted use case of AI deployment helping support hospitals.
Amigo AI, a “digital residency” for clinical AI, raised $11 million. Madrona led the round. Amigo notes it has completed 3 million patient encounters for customers that include Eucalptus, Diverge Health, and the Care Clinic. This appears to be a slight pivot from Amigo’s seed round, which General Catalyst led back in January 2025, when it was aimed at being a digital clone of experts.
Malama Health, a maternity care company for Medicaid, raised $9.2 million. Acumen America led the round. The round includes $2.3 million in an NIH grant and $1+ million in California state funding. Fierce Healthcare’s coverage is a nice overview of the model. Malama’s model centers around doulas, and it is in-network with Medicaid plans in California, Texas, and Colorado, with plans to move into VBC contracts. It partners with FQHCs and community health centers to refer patients into Malama’s program.
What I’m Reading
Healthcare Uses Specialized Language. It Needs Specialized AI, Too. by Amber Nigam and John Glaser
An interesting discussion about deploying large language models in healthcare and the implications of “doing no harm”. Read more
AI Won't Automatically Accelerate Clinical Trials by Ruxandra Teslo
A good perspective on the bottlenecks in designing better drugs and getting to therapeutic abundance. It highlights that AI is unlikely to shorten clinical trial timelines on its own, because the bottlenecks stem from operational and regulatory issues. Read more
This week on HTN
Community Brain Trust: Hims and Novo announce new partnership, members discuss the CMMI ACCESS webinar, how to prepare for an EHR migration, and more. Read here.
Weekly Health Policy Briefing: Bipartisan content with MA plans, a case study in work requirement implementation costs, and the twitchiness of ACA insurance investors. Read here.
Health Tech Nerds Radio
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.
