
D.C.
A brief from the bipartisan, congressional Joint Economic Committee (JEC) alleges that Medicare Advantage plans overpayments are driving up premium costs for all Medicare beneficiaries by “$212 per enrollee in 2025, totaling $13.4 billion in higher premiums.” While the report and its framing about upward pressure on individual premiums for MA and Original Medicare beneficiaries alike are novel, the findings are largely driven by MedPAC’s numbers, which the MA plans dispute.
It includes this incredibly compelling but perhaps slightly uncharitable chart showing the growth in incremental Part B premiums caused by these overpayments:
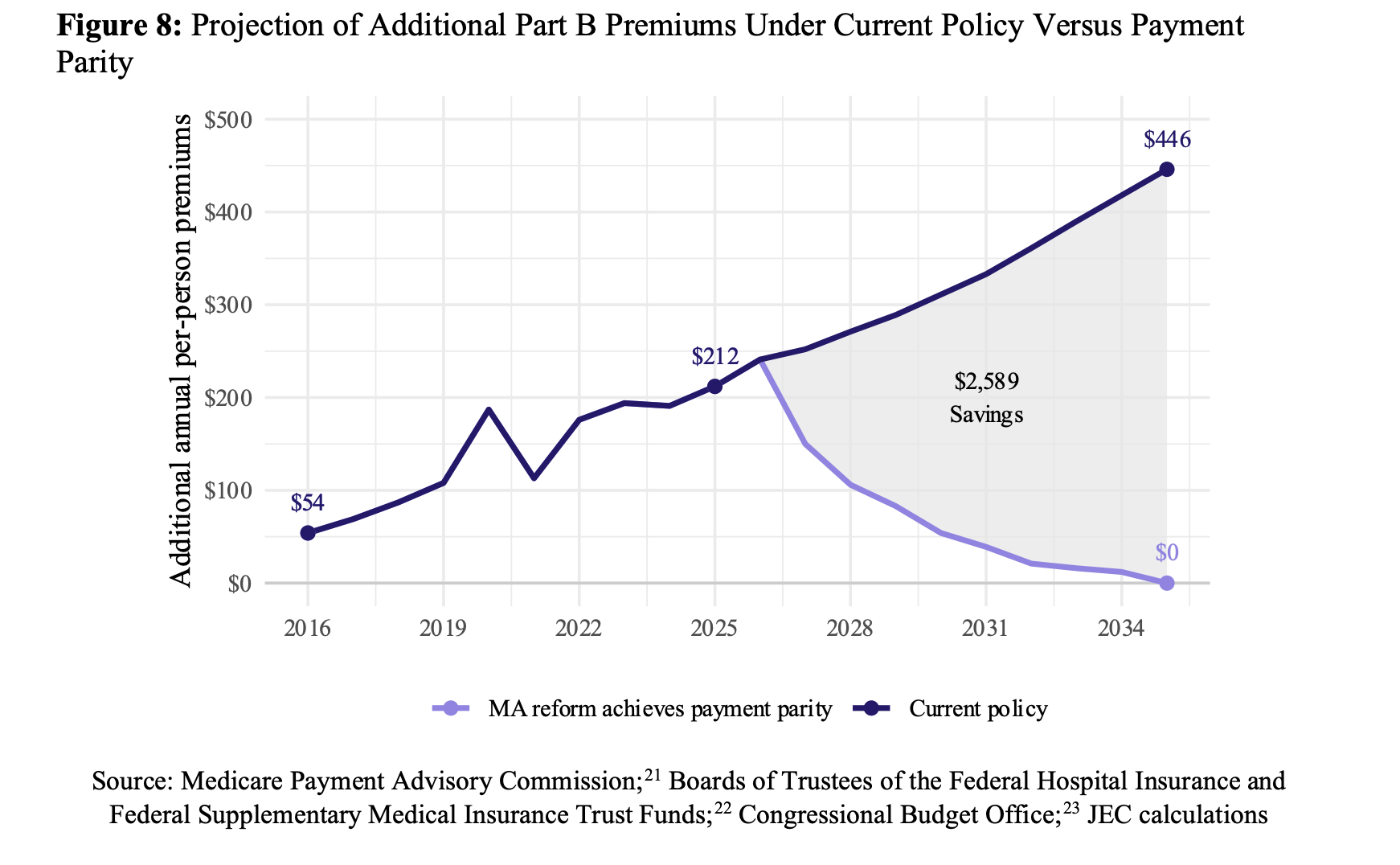
The way Part B premiums are calculated means that higher MA payments raise premiums across the board, so what the JEC is saying, despite the dispassionate bureaucratic language, is essentially, “those greedy MA plans are raising everyone’s premiums, whether you’ve got MA or Original Medicare.”
As we’ve talked about before, the question of what costs more, Original Medicare or Medicare Advantage, is largely unknown and potentially unknowable. MedPAC has a house view which is pretty well informed, but this paper from Yale’s recently formed Health Care Affordability Lab provides a nice synthesis of the academic literature on the subject.
The vaguely Solomonic finding of Zack Cooper et al. was that while MA does, in fact, spend less than Traditional Medicare, even after accounting for favorable selection, on a per-person basis due to care management, it costs the government more due to more generous benefits, coding practices, and risk adjustment.
Between this report, the impending final rate notice for 2027 which is expected to be unsatisfyingly low, and a recently announced ~$118m settlement from Aetna for False Claims Act allegations, one story you could tell is that the bipartisan consensus on Medicare Advantage is starting to crack. But my read of the situation is that it’s something closer to D.C. engineering a little creative destruction to get the program back to its roots in managing care and saving money.
Also in D.C., network-less health plans for the ACA, hospice fraud, the Cell and Gene Therapy Access Model, and an argument for abandoning high-deductible plans linked to spending accounts.
The States
Preparation for the implementation of the One Big Beautiful Bill is underway, with states and the District of Columbia getting the first tranche of federal funding to help them implement the new community engagement requirements. In total, states will get a little less than $2 million plus a 90% federal match for new system builds and 75% federal match for ongoing costs.
To give you a sense for what the state and federal government costs might net out to, we can look at the GAO’s review of Georgia’s 1115 waiver for implementing work requirements:
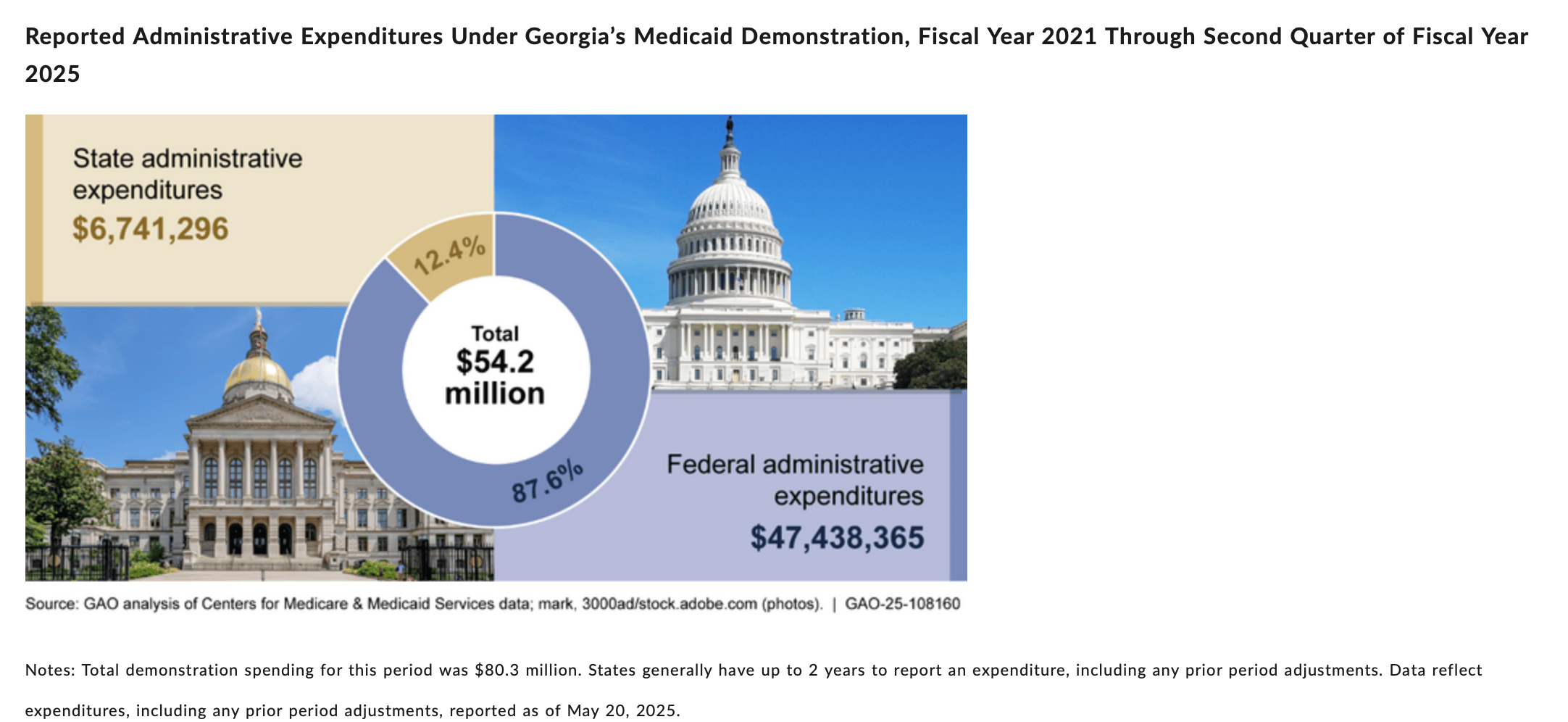
When Georgia applied for the waiver, it expected the program to be budget-neutral for the federal government, though, as the GAO points out, administrative costs aren’t part of CMS’s budget-neutrality considerations. It’s worth noting that the program has probably still netted out to savings for the taxpayers since enrollment has been both slower and lower than expected.
Also at the state level, despite not expanding Medicaid, Florida considers adding work requirements to their program, CMS gives states some options on the new eligibility check requirements, New Jersey approves a telehealth pilot for pregnant Medicaid members, Missouri is contemplating expanded prescribing privileges for NPs, an increasingly desperate Colorado budget situation leads to cuts for graduate medical education, and Tim Walz, Minnesota Governor, proposes stopping using Medicaid Managed Care organizations to administer the program and bring it all in-house.
The Private Sector
How many people are currently enrolled in Affordable Care Act Marketplace plans, colloquially known as Obamacare? The answer right now is that no one really knows. The official number from CMS is a little stale, from January 28th, but it had total enrollment at about 23 million people.
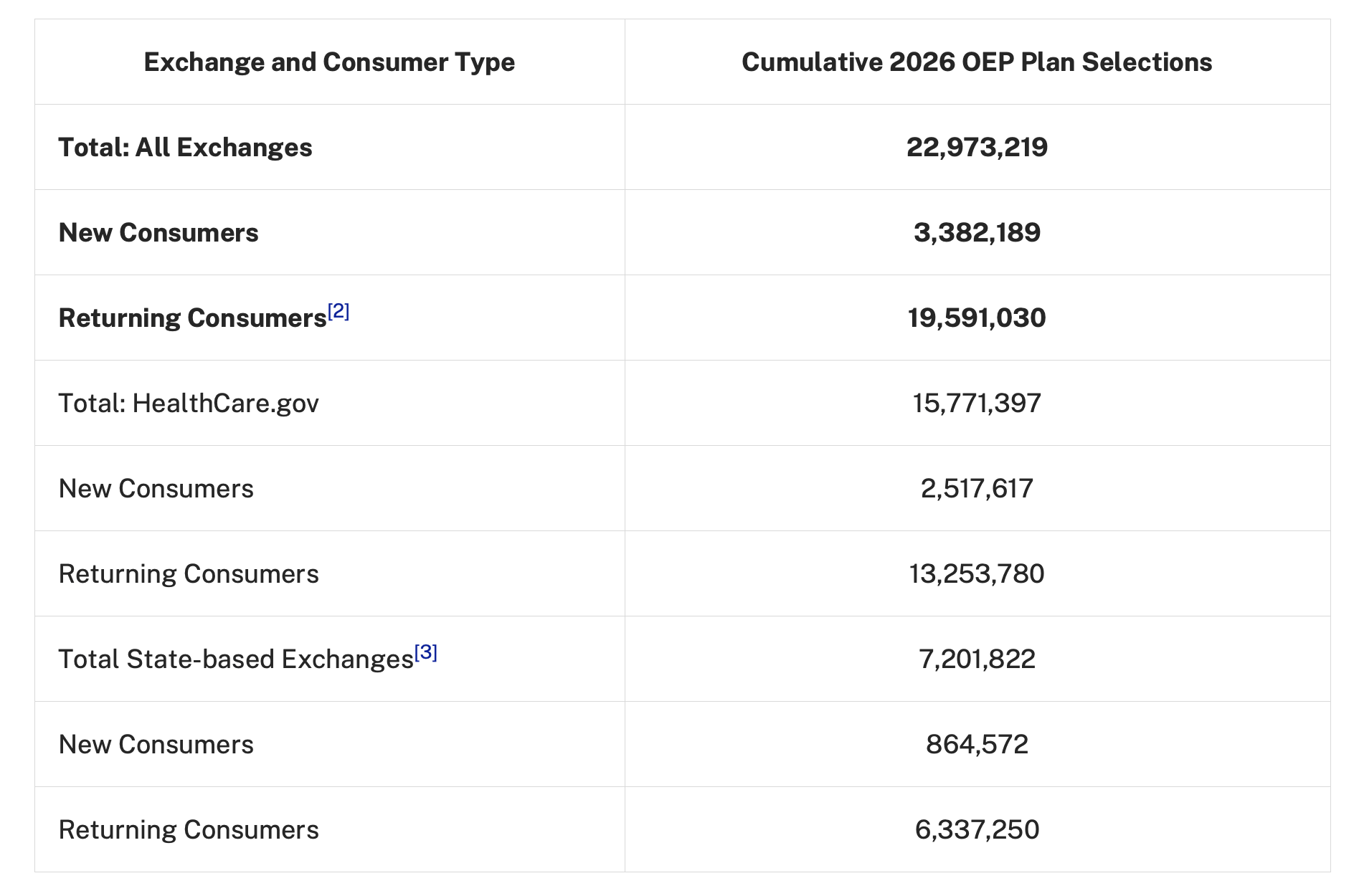
You shouldn’t over-index on the ~23 million number, though. Every year, regardless of what is going on, there’s a gap between an enrollment snapshot like this and the “effectuated enrollment” file that will be released by CMS later in the year. The gap between these numbers isn’t usually anything nefarious. Some people churn out because they get other, better insurance through an employer or qualify for Medicaid, but mostly, what happens is that some portion of the 23 million who chose a plan won’t end up paying their premiums.
Two things it’s important to note: first, there’s a 90-day grace period, so people who have opted into a plan but haven’t paid still have some time to settle their balances and keep their coverage. Second, if you look at the table above you’ll notice that a lot of the enrollees are returning customers, ~19 million. Many of these returning customers were automatically reenrolled in their current plan. As you may have heard, premiums are going up a lot year over year, so the worry is that some of these people who are automatically reenrolled are going to see the premium bill, chuck it in the garbage bin, and go uninsured.
Going uninsured didn’t used to be this frictionless because there was a penalty associated with not having insurance, but this was zeroed out during the first Trump administration. In the post-penalty version of the world, there tends to be some adverse selection. If you know you need insurance because, for instance, you have end-stage renal disease, you pay for it, and if you are reasonably certain you don’t need insurance, you don’t.
This makes it hard to price insurance accurately, and if you’re an investor in health insurance companies, you’d really like to know where enrollment is going to end up and, ideally, the nature of that enrollment, so you can have a better sense for what type of year the insurance companies you own are going to have.
This dynamic, marked by lots of uncertainty, has made everyone a bit jumpy. On Tuesday, Centene presented at an investor conference and shared that their ACA enrollment was stepping down in line with expectations, the stock dropped significantly and at time of writing is down ~17% on the week.
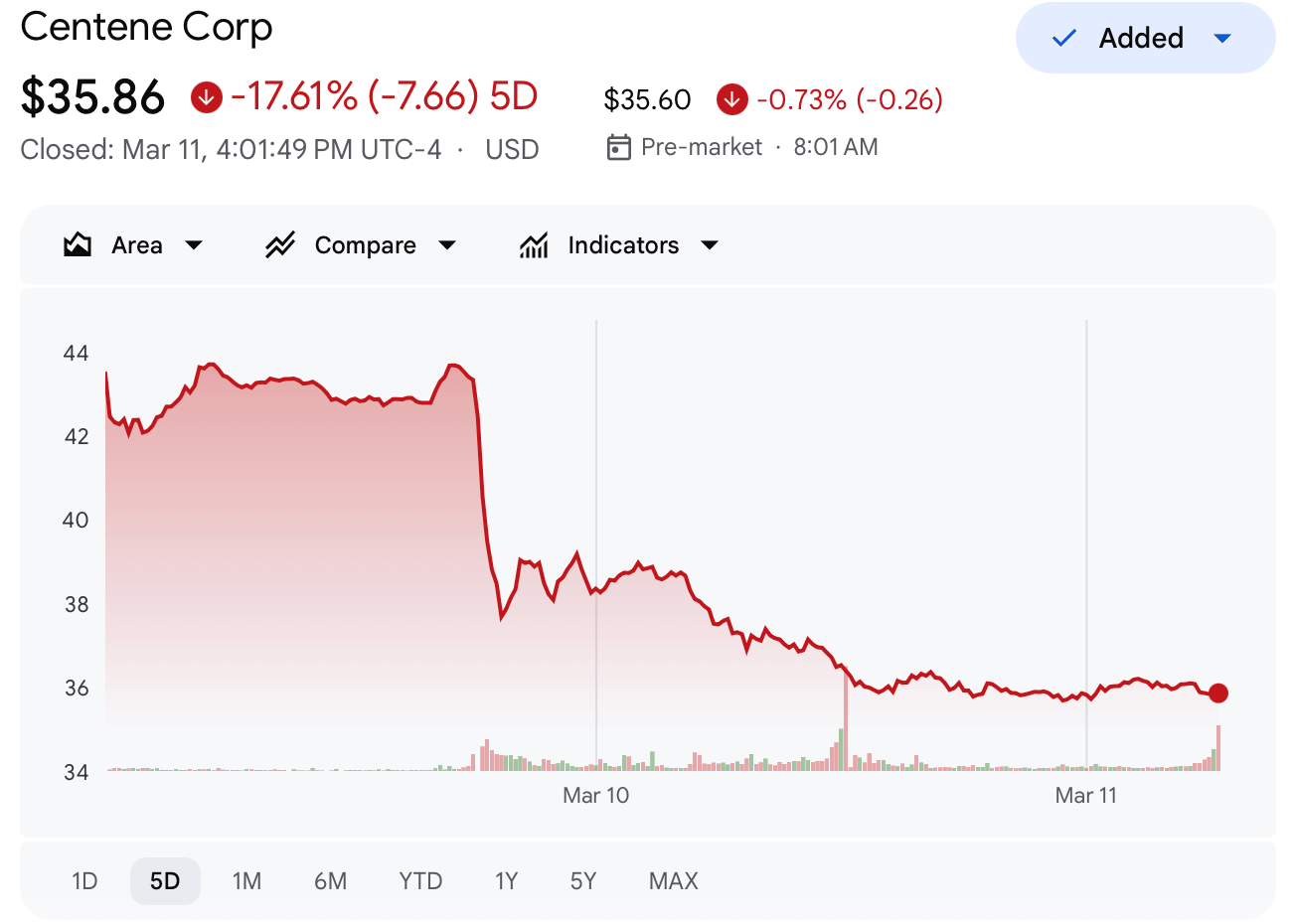
Oscar and Molina both saw big drops as well after Centene’s presentation, but have pared the losses. Elevance, which has some other stuff going on, shared a slightly different view of the market while reaffirming their floor of 900k members at year-end 2026 during the Barclays healthcare conference
Open enrollment activity came in stronger than we initially anticipated, with membership up approximately 10% sequentially. A meaningful portion of that growth was driven by our 2025 expansion states, specifically Texas and Florida, where we continue to see stronger traction. In our core blue states, membership trends were actually very much in line with the overall market. The key variable to your point here is effectuation rates, which is specifically how many members ultimately activate their coverage by paying their premiums. Through February, effectuation rates on both new sales and active renewals, they’re tracking in line with typical patterns.
I guess my question is what typical patterns? Non-effectuation rates have ranged from low single digits to double digits over the history of the program. My main takeaway here is that public market investors are a little jumpy at the moment, and there are a lot of different ways you could interpret softer enrollment or steeper non-effectuation than expected. At the conference, Centene said they priced for margin over growth, and the drop-offs were right where they thought they should be. Did they get adversely selected against or are they actually in a more profitable position? We won’t know until CMS releases effectuated enrollment details and Wakely releases their Marketplace risk adjustment data. In the meantime, I expect the volatility will persist.
Also, Health Enterprise Partners released their annual research survey, Nitra announces a blockbuster round, Sword enters the cardiometabolic space with an ACCESS-like fee scheme, hospital finance AI startup Translucent announces a Series A, Hims and Novo make nice, hospital operator UHS acquires Talkspace expanding their behavioral health reach, and the WSJ looks at the business of autism therapy.
More from Health Tech Nerds
Weekly Health Tech Reads: Musing about the coming tidal wave of CGTs, Emergency department disputes, a new Hims / Novo partnership, CMS on AI adoption and deflationary payments, and more. Read here.
Community Brain Trust: Hims and Novo announce new partnership, members discuss the CMMI ACCESS webinar, how to prepare for an EHR migration, and more. Read here.
Health Tech Nerds Radio
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.
