
Sponsored by: Alumni Ventures
The Alumni Ventures Healthtech Syndicate gives individuals the opportunity to invest in health tech startups that are typically only accessible to institutional investors.
Members get:
1-2 curated health tech deals per month, co-invested alongside firms including Andreessen Horowitz, Khosla Ventures, and Sequoia.
Full diligence materials on each deal: financials, market analysis, and live discussion with the AV investment team.
No cost or obligation to join; invest only in deals that interest you.
$10K minimum per deal when you do invest.
Sign-up is quick and straightforward–learn more and join here.
Reminder: HTN is not affiliated with Alumni Ventures and does not provide investment advice.
If you're interested in sponsoring the newsletter, let us know!
👋 Welcome to my Sunday recap of healthcare news. Welcome back after a week off! I spent a lot of time thinking this week about the journey to the 2027 Final Notice rate — including a fun interview with Chris Klomp — and what that implies for the industry ahead. It was interesting to read the downcoding lawsuit that Jefferson brought against Aetna this week against that backdrop. I’ll discuss all of that, along with Minnesotans’ affinity for Life Time memberships, and much more below. Enjoy!
- Kevin
TOP HEADLINE
2027 MA Final Notice comes in ahead of expectations
On Monday afternoon, CMS released its 2027 Final Notice, also known as the Calendar Year (CY) 2027 Medicare Advantage (MA) and Part D Rate Announcement. The headline was that the final Overall Expected Change came in above expectations at 2.48%, a meaningful increase from the 0.09% that was originally proposed in the Advance Notice.
This news sent Medicare Advantage stocks higher across the board, with many companies trading up ~10% on the week. I had the chance to sit down with Chris earlier this week and hear directly from him what CMS is thinking about as it finalized this rate:
Watch on: Apple. Spotify. YouTube. Or read the transcript here.
As I listen to Klomp explain the changes from the Advance Notice to the Final Notice, my mind can’t help but wander to a related story from my local newspaper this past weekend, discussing the operating losses that Blue Cross Blue Shield of Minnesota faced in 2025. It featured this photo of a group of ~50 seniors picketing BCBS MN headquarters in December because BCBS MN dropped free access to YMCA and Life Time gyms as part of its fitness benefit:
Now, as we discussed in Slack this week, if you know Minnesotans, you know we love our local brands. Life Time is right at the top of that list. I was actually just talking to a family friend last week who was lamenting this very issue as part of her frustration with insurers. She previously had MA coverage via UCare, loved her free access to Life Time, and was upset she lost it with BCBS MN. I’m pretty sure this is how the average American thinks about Medicare Advantage.
I’d imagine that many of the 44,000+ comments that CMS received after the Advance Notice shared in some form that the benefit cuts necessary to adjust to the rate increase contemplated in the Advance Notice would be fairly draconian, and that there might be a few more Minnesotans picketing in the streets over cuts.
Given that, the Final Notice seemed to land in a very reasonable spot, adjusting to ensure stability for beneficiaries in 2027 while also making it clear to the industry that CMS is serious about being better stewards of taxpayer dollars.
With the slightly favorable outcome providing clarity on 2027 expectations, much of the industry reaction focused on the implications for 2028 and beyond. Does a one-year delay in risk adjustment changes just mean this will show up as a headwind for the industry in 2028? Again, listening to Klomp talk about what CMS is trying to accomplish, I actually think the general trajectory here is pretty clear. Klomp mentioned during the conversation that the Final Notice rate came in roughly in line with GDP growth, and his view that outcome is reasonable as a growth rate for the industry. To me, that seems like the starting point when considering what to expect in 2028 and beyond. Within that, topics like risk adjustment changes seem like levers CMS knows it can and will pull, if needed.
If that is all right, I think the most interesting question coming out of this rate notice exercise isn’t risk adjustment, but rather how the industry will bring that medical cost trend number under control moving forward. If underlying medical costs are increasing at 5%+ per year and GDP is increasing at 3% a year, that math obviously isn’t going to work for CMS to hit its target of rates growing with GDP.
Navigating how to close that gap seems like the key question at hand for both CMS and the industry as a whole, and I think Klomp’s commentary provides a good sense of where the answer may lie from the CMS perspective, specifically around both payors and health systems needing to better control costs, the role of accountable care relationships, and ACCESS as a deflationary payment mechanism.
MUSING
The latest in payor/provider spats: Jefferson Health sues Aetna over two midnight rule downcoding
Jefferson Health filed a lawsuit against Aetna earlier this week, frustrated with Aetna’s new-ish payment policy change related to the Two Midnight rule. Aetna is now “downcoding” care it deems to be of lower severity. Jefferson argues that Aetna is changing the terms of its contract and shouldn’t be able to do so. To make the point, Jefferson presents the case below of a patient who was deemed low severity, which seems like a bad look for Aetna.

Yet while the case seems to me that it may have merit, it doesn’t explain why Aetna decided to implement this policy in the first place. Let’s assume for a second that Aetna was acting rationally in implementing this policy. Why put in place a policy like this? I’d be willing to wager it is because Aetna has data showing providers were perhaps taking advantage of the Two Midnight rule to get paid at inpatient rates for care that might otherwise have been paid at a lower rate. The only good reason I can think of for implementing a policy like this and risking provider abrasion is if it is a response to meaningful spending increases.
Stepping back from the specific merits of the case at hand, it strikes me as a good case study of how the tit-for-tat battle between payors and providers increases overall waste in the system. Both sides are capable of making good cases that the other is at fault and they are in the right, which IMO is largely a result of how you frame the specifics of the argument at hand.
As I shared in the Slack thread on Friday, I when I think about a case like this in the context of the broader discussion above about getting medical cost trend in line with GDP, I can’t help but feel like this is a bit like two children arguing over who gets the TV remote to pick what to watch next, not realizing their parent is coming over to take the remote away.
CHART OF THE WEEK
Teladoc’s BetterHelp Valuation Conundrum
Teladoc finds itself in an interesting strategic situation given its current valuation on the public markets. Last week, it received a letter from an activist shareholder arguing it is undervalued at the moment, largely due to a series of strategic mistakes over the last few years that have eroded investor confidence in the business. The investor is concerned that the current depressed valuation could encourage a takeover offer, and existing shareholders would miss out on the upside embedded in the business. Namely, it suggests a share buyback, cost-cutting, and a strategic review of BetterHelp as key exercises moving forward.
Then this week, Saki Georgiadis penned a great read on Substack, diving into the financial opportunity embedded within BetterHelp. It makes the case that BetterHelp is worth ~$1 billion today based on its insurance business, making a very similar point about Teladoc's valuation. He also suggests that if Teladoc sells BetterHelp for $1 billion, the remaining business should be worth ~$3.6 billion in total, versus the $1.24 billion the entire business is worth today:
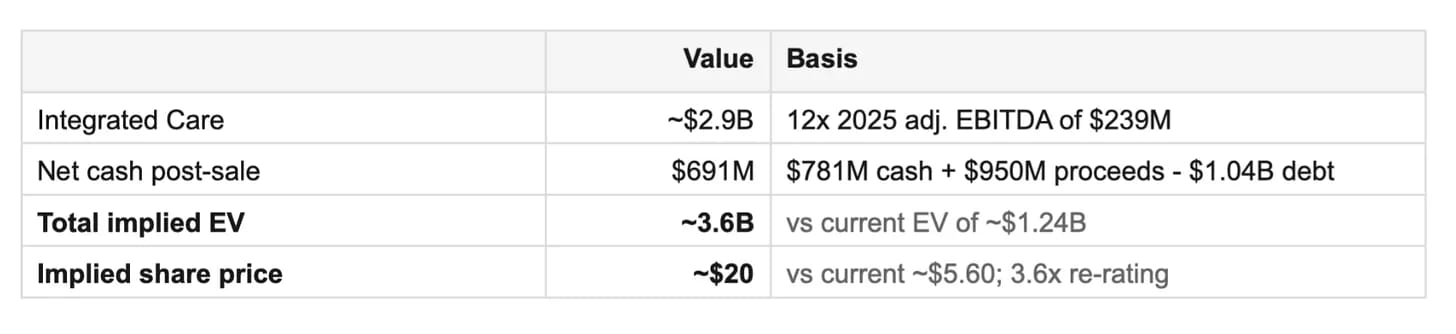
At these valuations, it seems like the logical conclusion is that BetterHelp will likely be a standalone business in the near future. As Georgiadis’s article notes, it’ll be worth keeping an eye on Q1 earnings and if the insurance business revenue is tracking to expectations.
A NUMBER TO PONDER
Humana’s VBC membership
71%
Humana released its latest annual report on the state of VBC. Kudos to them for keeping up with this report, even if it is not quite what it once was at peak-global cap. Humana reported that 71% of its individual MA membership is in VBC contracts (per its definition of VBC, which ranges from global cap to quality bonuses with no shared savings). The percentage membership in VBC contracts is up slightly from 68% in the 2022 report and 66% in the 2017 report. I find it fascinating to think about the types of contracts that make up this number over time, and how the global cap, in particular, has likely trended in recent years.
An interesting note on the opportunity in rural VBC: Humana noted that 75% of its urban members are aligned with a VBC PCP, while only 54% of its rural members are aligned with a VBC PCP. And that rural number is apparently up 19% since 2020 per the report.
Other Top Headlines
CMS released another major set of reforms on Friday evening, with tentacles across interoperability and other areas. Of particular note is the proposed CJR-X model, an expansion of the existing CJR model to make it mandatory and nationwide. A mandatory, nationwide bundle here seems like a big move from CMS.
Here in Minnesota, BCBS MN reports that it expects losses in 2026 as it manages an influx of Medicare Advantage membership after UCare left the market. BCBS MN reported a $353 million operating loss in 2025, which includes a $150 million premium deficiency reserve for ongoing losses. Note that overall, BCBS MN still turned a $83 million profit in 2025 based on its investment portfolio returns. BCBS MN highlighted inpatient care, specialty medications, and GLP-1s as key drivers of losses. As highlighted above, seniors in Minnesota are unhappy with the benefit cuts associated with these issues.
The Doctronic AI pilot in Utah has apparently caused significant concern with members of the state Medical Board, per Brian Dolan’s excellent reporting in the Exits and Outcomes newsletter on Friday. Dolan obtained correspondence among the Medical Board, the Pharmacy Board, and the Office of AI Policy, providing a glimpse into what feels like a chaotic process in Utah. If you’re at all interested in the adoption of AI in clinical settings, it is fascinating to see the back-and-forth here and to think about the implications for other states considering similar programs. It seems like you can see party lines emerging in these sorts of narratives — insurgents arguing that Medical Boards are protecting incumbent interests over patients, incumbents arguing that insurgents are risking patient safety. As always, it strikes me that there is merit to each argument, though it seems pretty clear to me which one is the winning argument politically — I think pissing off the state Medical Board is a losing battle.
Featured Jobs
Director, Program Growth & Operations at Cofertility, a fertility and family planning company. Learn more.
Remote
Vice President of Operations at Greenbrook Medical, a senior-focused primary care provider. Learn more.
Remote or Hybrid (Florida)
Associate Director Enterprise Strategy & Partnerships at UnitedHealth Group, a healthcare conglomerate. Learn more.
$112K - $193K | Remote
Director, Strategy & Operations at SmarterDx, an AI revenue integrity solution for hospitals. Learn more.
$170K - $190K | Remote
Applied AI Operations Lead at Canvas Medical, a customizable EMR for specialty care. Learn more.
SF (Preferred) or Remote
Contact us to feature roles in our newsletter.
Funding Announcements
Chapter, a Medicare brokerage/navigation platform, raised $100 million at a $3 billion valuation. Generation Investment Management led the round. Chapter reported tripling revenue and hitting $100 million of ARR in 2025, while keeping headcount flat. As noted in “What I’m Reading” below, the shifting Medicare landscape (coupled with AI) seems to be opening a window for brokerages at the moment.
Luminai, an AI platform for healthcare operations, raised $38 million. Peak XV Partners led the round. Luminai also announced it has partnered with the Cleveland Clinic to reduce administrative burden, with the first use case focused on referral management. Going back to the Cleveland Clinic’s JPM presentation, it highlighted its AI efforts with four core AI partners: Bayseian Health, Ambience Healthcare, Palantir, and Akasa. I count at least a few organizations in that list that I think would suggest they are helping the Cleveland Clinic with AI operations. Interesting to think about how this market evolves over time.
Yuzu, a TPA model supporting alternative plan designs, raised $35 million. General Catalyst and Chemistry led the round. If you’re curious what a TPA for alternative plan designs looks like, we spent time with one of Yuzu’s co-founders unpacking this topic a few months ago.
Jimini Health, a behavioral health AI model, raised $17 million. Investors included Town Hall Ventures, which shared its investment thesis. Jimini is building a mental health chatbot, Sage, that operates as an extension of clinicians to help them scale capacity.
Insight, a clinical voice AI company, raised $11 million. Standard Capital led the round. The press release states that Insight has saved more than $50 million in administrative costs for clients, including The Oregon Clinic, Pacific Sports & Spine, Inland Neurosurgery, Coastal Health, and Santiam Hospital.
SimpliFed, a virtual maternal health platform, raised $10 million. Morningside and Hesperia Capital led the round. SimpliFed is in-network with most commercial plans and Medicaid in several states. We’ll be chatting with Andrea about SimpliFed on The Grand Round Up tomorrow.
What I’m Reading
He Was an Insurance Executive. She’s a Doctor. They’re Divided. by Elisabeth Potter and Troyen Brennan
I thought this was a well-done conversation in the New York Times, bringing together Elisabeth Potter, the Texas-based doctor famous for her issues with insurance companies, and Troyen Brennan, formerly the CMO at CVS. As we discussed in Slack this week, while I think Potter makes a number of reasonable points that tend to win over the average listener, I think Brennan makes a much more coherent, nuanced set of points that grapples more directly with the challenges facing the system. Read more
The Most Responsible Path in Healthcare AI Is Also the Deadliest by Giovanni Colella
Colella highlights the story of shuttered mental health AI startup Kintsugi and the issues it faced in trying to build healthcare AI by the book. Ultimately, Kintsugi spent 7 years and $30 million before winding down and, unfortunately, becoming a really good case study in the challenges of healthcare AI. As folks in DC think about creating a level playing field for insurgents to disrupt the industry, a journey like this poses some good, and challenging, questions to grapple with. Read more
The MEDVi Files by Brendan Keeler
The MEDVi story obviously caught the attention of social media this week. I thought this analysis by Brendan Keeler was the most interesting I read, highlighting how the story seems like a sign of the times for a part of the industry that feels a bit like a gold rush at the moment. It’s fascinating to juxtapose the MEDVi story with the Kintsugi story above when contemplating the behaviors we want to support from a regulatory perspective. It all feels backward to me at the moment, personally, but it's worth keeping in mind that innovators are always out in front of regulatory change.
Read more
Why Are People Injecting Themselves with Peptides? by Dhruv Khullar
On the topic of gold rushes, I thought this read on the peptide craze was excellent. The example of the Charleston doctor making tens of millions of dollars a year running a longevity clinic is great, particularly the discussion of how the doctor evaluates anecdotal data on peptide shots versus studies of COVID-19 vaccines. Read more
The CEO of UnitedHealthcare on Fixing What Frustrates Customers Most by Tim Noel
An HBR article by UHC’s CEO, Tim Noel, discusses how UHC has built a Consumer Resolution Center that combines AI and human expertise to resolve issues for members in distress. The results cited are really impressive — serving 150,000+ members and raising their satisfaction scores from 0 out of 10 to 8.8 out of 10, with a spillover effect in which solving the root causes of those members' issues has improved the experience for 10% of UHC’s overall customer base. Well worth a read. Read more
UnitedHealth Group is making a $3 billion bet on AI. What does it mean for patients? by Casey Ross
This Stat article examines how UHG is working to deploy AI across the organization, highlighting the potential risks that AI could pose to patient safety. I find it interesting to read an article like this on the same week that the HBR article above was published. My personal answer to the question posed in the Stat headline is that UHG's use of AI actually seems like a good thing for patients! UHC’s CRC seems like a very tangible example of that. Read more
Positioning for Leadership in Medicare Advantage Brokerage by Patrick Keavy, Rebecca Springer, and Collin Anderson
A Bailey & Co. report on the MA brokerage market highlights the potential for consolidation ahead. It’s fascinating to think about the role brokerages will play going forward in an MA market that is seeing margin compression. While that could lead to compression in commissions, it could also create more opportunities for brokers who drive improved engagement and retention for plans. Read more
Blues Plans Are Consolidating From Within. Your Pipeline May Not Reflect It Yet. by Ryan Peterson
An interesting look at the current state of Blues plan consolidation. It makes the point that the Second Blue Bid process is going to speed up consolidation in this market, which is an angle I hadn’t thought through previously, but makes a ton of sense to me. Read more
The great unbundling by Neel Shah
A good perspective on how maternity care will be paid for differently starting January 1st, 2027, as changes to CPT Codes will unbundle maternity care into a series of separate charges. Unsurprisingly, lots of potential downstream implications to think through.
Read more
HTN Content From the Week
Want to comment or share feedback?
If this newsletter was forwarded to you, subscribe here or see more from Health Tech Nerds.


