🧵TOP THREADS OF THE WEEK
In case you missed them, here are highlights of a few interesting conversations from different channels:
Threads included below:
Clinical supervision of PAs & NPs
Watchouts with RPA bot web-scraping
Understanding the risks of online tracking technologies
Eye tracking tech for pediatric autism & ADHD
Unpacking insurance company network discrepancies
1. Clinical supervision of PAs & NPs
Q: clinical supervision of PAs and NPs
it seems that supervision requirements for PAs and NPs have gotten more and more relaxed. for example, fewer and fewer states are requiring cosignature of notes. what do other virtual care organizations require for PA (and NP) supervision? does this change over time as a PA, for example, is in the organization for longer? specifically:
- cosignatory of notes
- sync meetings
- other
– Grace Hunter| via #buildersask
Thread Summary: Several clinicians discuss best practices and state laws regarding clinical supervision of PAs and NPs in the US.
Top Response:
Desmond Watt: To me it’s about finding the right balance between compliance with state rules and offering meaningful collaboration for clinicians. If your program is just a box checker, you’re missing an opportunity for clinicians to better understand each other and their patients.
We’re in all 50 states, so we’re intimately familiar with the complexity of negotiating variable state practice rules. We tend to cohort clinicians to a cluster of states where they can most effectively operationalize collaboration requirements, and we cross-license physicians for collaboration where required to simplify the process (as opposed to PAs and NPs working with multiple collab docs state by state).
Frankly my question continues to come down to: in a world where all clinicians have full practice authority, do we still collaborate? Yes - of course. With that in mind - what is that model, and how can your current system enable something as close to that as possible, while remaining compliant with state rules.
Speaking personally as a PA, I’ve been disappointed in seeing the number of telehealth companies who seem to want to take the “easy route” by completely excluding PAs from hiring in favor of NPs who have full practice in 26 states. PAs are outstanding clinicians with excellent and standardized training regimens. The complexity of collaboration can be easily addressed with a thoughtful program.
Folks like @Rafid Fadul likely have some thoughts on this as well from the physician perspective.
2. Watchouts with RPA bot web-scraping
Q: I know some of ya'll use RPA bots to scrape web-based EHR data. Are violations of ToS a concern?
– Aditya Singh | via #buildersask
Thread Summary: The crew shares advice and past experiences from other EHR orgs on potential risks and watchouts when leveraging RPA bots to scrape web-based EHR data.
Top Response:
Jonathan Meneses: Also worked at an EHR:
We knew it was happening and it wasn't great, but we didn't have much ability to stop it. Saying it's against ToS was more our way of saying "hey we can't support you if something goes wild because this is out of our scope of support"
As a client of EHRs, I've had a couple recommend RPA to me when their functionality was lacking (particularly in automation and reporting). When I asked if that was against their ToS, I got an answer that was pretty much "well... yeah, but we aren't going to do anything about it"
I would expect if you're employing RPA to get around paying a fee to an EHR, they'll be motivated to shut it down. If there's functionality that is missing that RPA or some process provides, I wouldn't really be that worried, as long as you have appropriate safeguards in to protect sensitive data in place
3. Understanding the risks of online tracking technologies
Q: How are people thinking about this? Is everyone off google/fb?
FTC and HHS Warn Hospital Systems and Telehealth Providers about Privacy and Security Risks from Online Tracking Technologies [Link]
– Jenni Friedman | via #topic-marketing
Thread Summary: An insightful thread unpacking implications of a recent joint statement from the FTC and HHS health systems and telehealth providers about security risks from online tracking technologies.
Top Response:
Chris Turitzin: I've been personally tracking a set of virtual care companies and their usage of trackers for about a year now. What I'm seeing:
1. Prominent "condition specific" companies in sensitive verticals have mostly all removed trackers. (they have at least removed JavaScript based trackers, I don't know if there is a way of knowing if they are still using server side trackers)
2. Prominent multi-condition companies (e.g.. generic mental health) have reduced tracker usage, but some still use them. Some have removed entirely.
3. Smaller condition specific companies (either because they are new or not "VC path") are in large part still using trackers.
4. Eye tracking tech for pediatric autism & ADHD
Q: Saw this article today on Autism diagnoses using eye tracking.
One of the most important advantages of this software is its capacity to detect autism early, allowing for earlier intervention and treatment. Early intervention has been demonstrated to enhance outcomes for autistic children, reducing the need for long-term assistance and boosting the quality of life.
It reminds me of what @Adi Diner is working on with ADHD. I’m curious how those who are operating more of the pediatrician/primary care are thinking about partnerships / usage of this type of technology in your workflows / patient journeys, if at all? (@Ellen DaSilva and others..)
– Ryan Russell | via #topic-pediatrics
Thread Summary: A group of HTNers in the peds space chat about partnership opportunities to leverage technologies such as eye tracking in the patient journey for autism and ADHD.
Top Response:
Ellen DaSilva: Interesting article @Ryan Russell (HTN Team)! We have thought a bit about early intervention and early treatment. My general sense is that primary care isn't suited for this given how infrequently people access their PCP, even for pediatrics. I could see a place like Summer Health leaning in here because we treat your kids 1-2x per month rather than the 1x well visit per year. This needs some more frequent tracking. Might be harder via telehealth, though.
5. Unpacking insurance company network discrepancies
Q: Does anyone have any idea how/why an insurance company could say a provider is in-network but then after filing a claim, it turns out that the provider is out of network?
Have a dermatologist who says that even though insurance directories say they’re in network for Empire BCBS Gold/Silver/Bronze plans, all of a sudden last December, they started to notice that these plans were actually being treated as OON. Same thing with United Metro/Liberty/Advantage.
For one BCBS Gold member, we even after called insurance to verify and they said the provider is in network, so I’m not sure how possible/frequent it can be that insurance is wrong in determining in/out of network status?
– Kevin Chiu | via #topic-rev-cycle-management
Thread Summary: A few HTNers detail several explanations for why an insurance company may have provider network discrepancies before and after claims fillings.
Top Response:
Duncan Reece: It can be many things. provider directories are a massive mess
1. provider is in network for some plans within the org and not others
2. provider is in network for some services and not others
3. contract termed and directory is not updated
4. data issue
5. member is not actually covered
6. etc. etc.
unfortunately to understand you need to get in the weeds with the insurance company
❓UNANSWERED ASK
Here we highlight a question from the Slack that needs some additional community insights - if you have a helpful thought, jump in below!
Q: Hi folks, I'm at a telehealth company and we're starting to submit Medicare enrollment applications. How does Medicare reimburse telehealth for out of state providers? For example, let's say we enroll in Medicare jurisdiction J5 (which includes MO, KS, NE, and IA) with a Missouri address, then we submit a telehealth claim for a patient in Kansas (assume the provider is licensed in KS). How would we get reimbursed, what rates would be used? Thanks in advance for your help!
– Katy Henrickson | via #buildersask
🤖HTN KNOWLEDGE BOT
If you have your own question(s) to ask, don’t forget that a good place to start is our HTN Knowledge Bot. It’s our smart search tool that makes it easier to access the wisdom shared within the HTN powered by ChatGPT. You can log in and use it on the website (here) or see how to use it directly in Slack here.
Check out the example ask below!
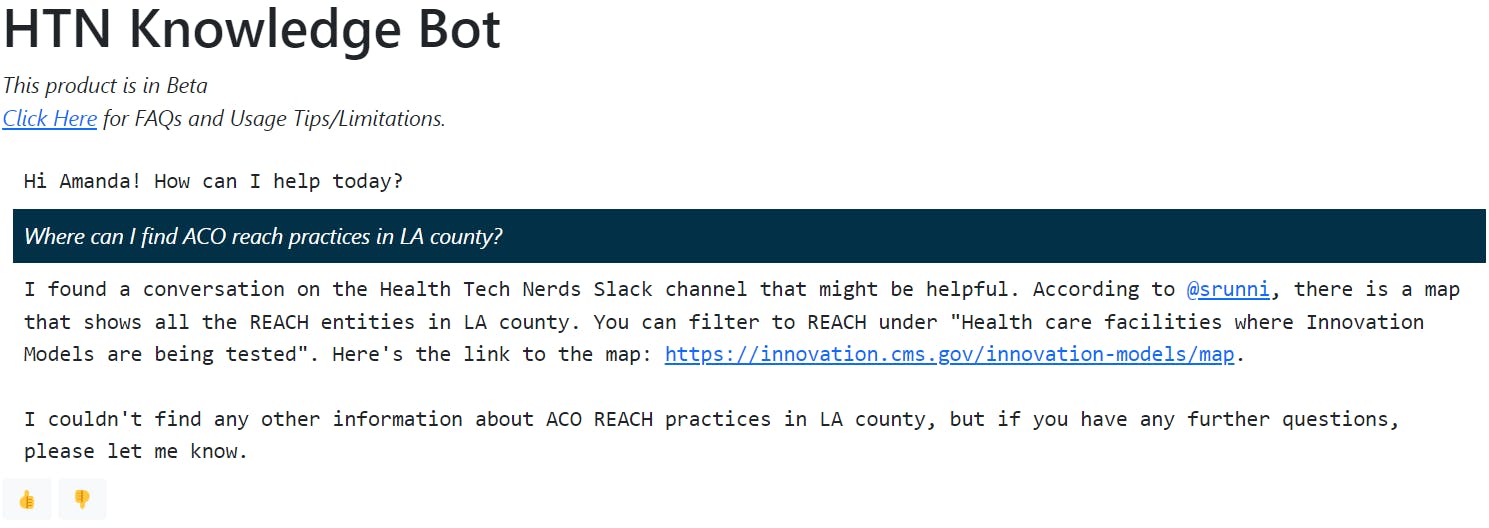
Here we highlight helpful resources from across the community:
Data sources for claims-based analysis via Tamra Lair – A working list of data sources for claims analysis.
US Healthcare 101 Study Guide by Lukas Steinbock – A 101 explainer of various healthcare topics.
Prompt Engineering Guide via Brian Dailey – A Notion guide to ChatGPT prompt engineering.
The Intersection of AI and ADHD by Adi Diner – An interesting article discussing the intersection of AI and ADHD.
Part 1: So you want to buy a healthcare service business... by Zach Miller – Part 1 of a three part series on the nuts and bolts of private equity in healthcare.
Health Tech Topics Table of Contents by Ben Clark – A collection of 34 articles on health tech and the major players in the space.
Pitch Collective via Evan Brociner – A group of VCs is hosting a virtual pitch event for B2B software companies with <$500K of raised capital.
New England Journal of Medicine AI Journal via Jake Fishbein – NEJM is launching a brand new AI-focused journal.